Cholesterol/HDL Ratio: A Better Predictor of Heart Disease Risk Than Total Cholesterol
Why your cholesterol ratio matters more than your total cholesterol number
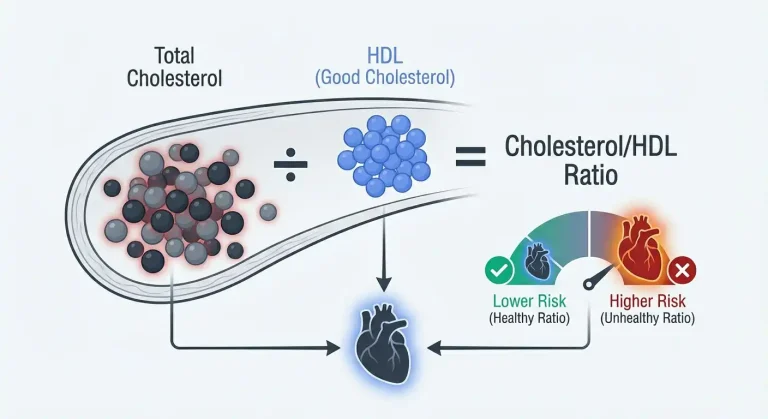
What Is the Cholesterol/HDL Ratio?
The cholesterol/HDL ratio is a simple calculation that compares your total cholesterol to your HDL cholesterol (the “good” cholesterol). This ratio provides a far more accurate assessment of cardiovascular disease risk than total cholesterol alone, yet many doctors still focus primarily on the total cholesterol number while ignoring this critical metric.
The calculation is straightforward: divide your total cholesterol by your HDL cholesterol. For example, if your total cholesterol is 200 mg/dL and your HDL is 50 mg/dL, your ratio is 4.0 (200 ÷ 50 = 4.0).
This simple number tells you more about your actual heart disease risk than knowing your total cholesterol in isolation. You can have “high” total cholesterol but excellent cardiovascular health if your HDL is proportionally high. Conversely, you can have “normal” total cholesterol but elevated risk if your HDL is too low.
Understanding this ratio shifts focus from the outdated “lower cholesterol at all costs” mentality to a more nuanced view of lipid health. Your body needs cholesterol for hormone production, cell membrane integrity, vitamin D synthesis, and countless other vital functions. The question isn’t whether your cholesterol is high or low, it’s whether you have the right balance between protective HDL and potentially problematic lipoproteins.
Why the Cholesterol/HDL Ratio Matters for Heart Health
Cardiovascular disease remains the leading cause of death globally, and lipid management is central to prevention. But decades of focusing solely on lowering total cholesterol has led to oversimplified (and often incorrect) approaches to heart health.
Total cholesterol tells you almost nothing about risk in isolation. You could have total cholesterol of 250 mg/dL and be at low risk if your HDL is 80 mg/dL (ratio of 3.1). Or you could have total cholesterol of 180 mg/dL and be at elevated risk if your HDL is only 30 mg/dL (ratio of 6.0). The ratio accounts for this critical context that the total number misses entirely.
HDL cholesterol is protective because it performs reverse cholesterol transport. HDL particles travel through your bloodstream picking up excess cholesterol from arterial walls and other tissues, transporting it back to your liver for processing and elimination. Higher HDL means more efficient removal of cholesterol from places where it can cause problems.
The ratio captures the balance between total cholesterol (which includes both protective and potentially harmful lipoproteins) and HDL (the protective component). A lower ratio indicates you have more of the protective HDL relative to total cholesterol, suggesting better cardiovascular health. A higher ratio means you have less protective HDL relative to total cholesterol, indicating elevated risk.
Multiple studies have demonstrated that the cholesterol/HDL ratio predicts cardiovascular events more accurately than total cholesterol, LDL cholesterol, or triglycerides alone. It’s a simple metric that captures complex lipid dynamics in a single number that correlates strongly with actual heart attack and stroke risk.
Normal vs. Optimal Cholesterol/HDL Ratio
Understanding where your ratio falls on the risk spectrum is essential for cardiovascular optimization.
Standard Risk Categories
Most guidelines categorize cholesterol/HDL ratios as follows:
Less than 3.5: Optimal. This indicates you have abundant protective HDL relative to total cholesterol, suggesting low cardiovascular risk.
3.5 to 5.0: Average risk. This is where most people fall, but “average” doesn’t mean optimal, especially for high performers focused on longevity.
5.0 to 6.0: Elevated risk. This ratio suggests insufficient HDL relative to total cholesterol, indicating increased cardiovascular disease risk.
Greater than 6.0: High risk. This represents significantly elevated cardiovascular risk requiring intervention.
The Problem With “Average”
A ratio of 4.5 might be flagged as “within normal limits” by your doctor, but it still indicates elevated risk compared to optimal. The goal isn’t avoiding the worst outcomes, it’s achieving the best cardiovascular health possible for long-term performance and longevity.
Optimal Range for Performance and Longevity
For high performers focused on cardiovascular optimization:
Optimal: Less than 3.0. This indicates excellent lipid balance with abundant protective HDL.
Good: 3.0 to 3.5. Solid cardiovascular health with room for improvement.
Needs improvement: 3.5 to 5.0. Not immediately dangerous but suboptimal for long-term health.
Requires intervention: Greater than 5.0. Elevated cardiovascular risk that demands action.
The difference between a ratio of 4.5 (average) and 2.5 (optimal) can represent decades of additional healthspan. Cardiovascular disease develops over decades. Optimizing your ratio now prevents the arterial damage and plaque formation that leads to heart attacks and strokes in your 50s, 60s, and beyond.
What Your Cholesterol/HDL Ratio Reveals About Cardiovascular Risk
The ratio provides insight into several aspects of cardiovascular health that individual cholesterol numbers miss.
Arterial Health and Plaque Formation
A high ratio (low HDL relative to total cholesterol) suggests inadequate reverse cholesterol transport. Cholesterol accumulates in arterial walls because you don’t have enough HDL particles to remove it efficiently. Over years and decades, this leads to atherosclerotic plaque formation, arterial stiffening, and eventually cardiovascular events.
A low ratio (high HDL relative to total cholesterol) indicates efficient cholesterol removal from arterial walls. Even if your total cholesterol is moderately elevated, abundant HDL provides significant protection by constantly clearing excess cholesterol before it can accumulate and cause damage.
Inflammatory Status
The cholesterol/HDL ratio often correlates with inflammatory markers. High ratios typically coincide with elevated inflammation, which accelerates atherosclerosis and increases plaque instability. Low ratios often coincide with lower inflammation and better overall metabolic health.
Metabolic Health
HDL levels (and thus your ratio) reflect metabolic health more broadly. Low HDL and high ratios are associated with insulin resistance, metabolic syndrome, and increased visceral fat. These metabolic dysfunctions drive cardiovascular disease through multiple pathways beyond just lipid imbalance.
High HDL and low ratios typically indicate good metabolic health, insulin sensitivity, and favorable body composition. The ratio serves as a simple marker for complex metabolic processes affecting cardiovascular risk.
Lipoprotein Particle Dynamics
While the basic cholesterol/HDL ratio doesn’t directly measure particle number or size, it provides clues about overall lipoprotein balance. High ratios often coincide with unfavorable particle profiles (more small dense LDL, fewer large HDL particles). Low ratios typically indicate better particle dynamics.
What Causes an Elevated Cholesterol/HDL Ratio?
Understanding root causes allows for targeted intervention rather than just treating numbers.
Low HDL Cholesterol
The most common cause of an elevated ratio is insufficient HDL. Even with normal or moderately elevated total cholesterol, low HDL creates a poor ratio. Several factors suppress HDL production and levels.
Sedentary lifestyle is one of the strongest predictors of low HDL. Physical inactivity reduces HDL levels substantially, while regular exercise (particularly aerobic exercise and high-intensity interval training) increases HDL production.
Smoking dramatically lowers HDL cholesterol. Even moderate smoking can reduce HDL by 10-15%, significantly worsening your ratio.
Excess body fat, particularly visceral adiposity (belly fat), suppresses HDL levels. The relationship is dose-dependent: more visceral fat correlates with lower HDL. This is independent of total body weight. You can have normal BMI but elevated visceral fat and low HDL.
High refined carbohydrate and sugar intake reduces HDL while elevating triglycerides. This dietary pattern creates the worst possible lipid profile for cardiovascular health.
Certain medications lower HDL, including beta blockers, benzodiazepines, and anabolic steroids. If you’re taking medications that suppress HDL, work with your physician on strategies to mitigate this effect.
Elevated Total Cholesterol
Sometimes the ratio is elevated because total cholesterol is too high relative to HDL, even if HDL is reasonable. This often reflects increased LDL cholesterol or elevated triglycerides (which contribute to total cholesterol calculation).
Dietary factors affecting total cholesterol are more nuanced than previously thought. For most people, dietary cholesterol and saturated fat have modest effects on blood cholesterol. Genetics, metabolic health, and overall dietary patterns matter more than individual nutrients.
Hypothyroidism (underactive thyroid) elevates LDL cholesterol and total cholesterol, worsening your ratio. Optimizing thyroid function often improves lipid profiles substantially.
Genetic factors play a significant role in cholesterol levels. Familial hypercholesterolemia causes very high LDL and total cholesterol from birth. Less severe genetic variations still influence your cholesterol levels and ratio substantially.
Combined Issues
Often, elevated ratios result from both low HDL and elevated total cholesterol simultaneously. This creates the worst cardiovascular risk profile. Addressing both components through comprehensive lifestyle optimization and potentially targeted interventions provides the best results.
Symptoms and Consequences of Poor Cholesterol/HDL Ratio
Unlike many health markers, an elevated cholesterol/HDL ratio produces no immediate symptoms. Cardiovascular disease develops silently over decades before symptoms appear. By the time you experience chest pain, shortness of breath, or other cardiac symptoms, significant arterial damage has already occurred.
Long-Term Consequences of Elevated Ratio
Atherosclerosis develops progressively as cholesterol accumulates in arterial walls, forming plaques that narrow blood vessels and reduce blood flow. This process begins in your 20s and 30s but doesn’t produce symptoms until arteries are significantly narrowed or plaques rupture, causing acute events.
Increased heart attack risk is the most obvious consequence. High cholesterol/HDL ratios predict myocardial infarction (heart attack) risk more accurately than most other lipid markers. The higher your ratio, the more likely you are to experience a cardiac event.
Stroke risk increases similarly. Atherosclerosis affects arteries throughout your body, including those supplying your brain. High ratios increase both ischemic stroke (from blocked arteries) and the consequences of hypertension.
Peripheral artery disease develops in leg and arm arteries, causing pain with exertion, poor wound healing, and eventual tissue damage if severe.
Erectile dysfunction often precedes cardiac events by several years. The small arteries supplying erectile tissue are affected by atherosclerosis earlier than larger coronary arteries. ED can be an early warning sign of systemic cardiovascular disease reflected in your cholesterol/HDL ratio.
The Silent Decades
The insidious nature of atherosclerosis means you feel fine while disease progresses. Your elevated ratio at age 35 produces no symptoms but predicts your heart attack risk at age 55. This is why optimization matters. Prevention requires addressing risk factors before symptoms develop, not after.
Testing Your Cholesterol/HDL Ratio
Understanding your ratio requires testing both total cholesterol and HDL cholesterol through standard lipid panels.
What’s Included in a Standard Lipid Panel
A basic lipid panel measures total cholesterol, HDL cholesterol, LDL cholesterol (usually calculated, not directly measured), and triglycerides. From these values, various ratios can be calculated, including cholesterol/HDL ratio.
Most doctors order lipid panels as part of routine health screening, but frequency varies. Annual testing is common, though more frequent testing may be appropriate if you’re optimizing cardiovascular health or tracking interventions.
Calculating Your Ratio
The calculation is simple: total cholesterol divided by HDL cholesterol. If your lab report doesn’t include the ratio automatically, calculate it yourself. For example, total cholesterol of 180 mg/dL divided by HDL of 60 mg/dL equals a ratio of 3.0.
Interpreting Results in Context
Your ratio should always be interpreted alongside other lipid markers and cardiovascular risk factors. A moderately elevated ratio with otherwise excellent health markers (low triglycerides, low inflammation, good metabolic health) carries different implications than the same ratio with multiple other risk factors.
Advanced lipid testing (particle number, particle size, lipoprotein subfractions) provides additional context but isn’t necessary for everyone. The basic cholesterol/HDL ratio captures most of what matters for cardiovascular risk assessment.
Testing Frequency for Optimization
If your ratio is optimal (less than 3.0) and stable, annual testing as part of comprehensive panels is sufficient. If your ratio is elevated or you’re implementing interventions, test every 3-6 months to track progress and adjust strategies based on response.
Improving Your Cholesterol/HDL Ratio
Optimizing your ratio requires addressing both components: raising HDL and, if necessary, managing total cholesterol. The strategies for improvement are well-established and highly effective for most people.
Increase Physical Activity
Exercise is the most powerful intervention for raising HDL cholesterol. Both aerobic exercise and resistance training improve HDL, with aerobic activity showing particularly strong effects.
Aim for at least 150 minutes of moderate-intensity aerobic exercise weekly, or 75 minutes of vigorous-intensity activity. More is generally better for HDL optimization. High-intensity interval training (HIIT) may be especially effective for raising HDL in time-efficient workouts.
Resistance training contributes to overall metabolic health and body composition, indirectly supporting better lipid profiles even if effects on HDL are more modest than aerobic exercise.
The key is consistency over time. HDL responds to regular ongoing activity, not sporadic intense efforts. Build sustainable exercise habits that you’ll maintain for years.
Optimize Body Composition
Reducing excess body fat, particularly visceral fat, improves HDL levels and your overall ratio. Even modest fat loss (5-10% of body weight) can significantly improve lipid profiles in those carrying excess fat.
The relationship between body composition and HDL is dose-dependent. More fat loss generally means better HDL improvements, though this plateaus at healthy body fat levels. You can’t exercise your way to infinitely higher HDL by becoming excessively lean.
Focus on sustainable approaches to body composition improvement through reasonable caloric balance, adequate protein intake, and consistent training rather than extreme dieting that’s impossible to maintain.
Improve Dietary Quality
While dietary cholesterol and saturated fat effects are more modest than once believed, overall dietary patterns significantly impact lipid profiles.
Reduce refined carbohydrates and added sugars. High sugar and refined carbohydrate intake lowers HDL while raising triglycerides, worsening your ratio from both directions.
Increase intake of healthy fats from sources like olive oil, avocados, nuts, and fatty fish. Omega-3 fatty acids from fish appear particularly beneficial for cardiovascular health and may modestly improve HDL.
Adequate protein intake supports satiety and body composition goals while providing building blocks for HDL particle production.
Focus on whole, minimally processed foods rather than obsessing over individual nutrients. Overall dietary patterns matter more than individual food choices.
Stop Smoking
If you smoke, quitting is one of the most impactful interventions for improving HDL and overall cardiovascular health. HDL typically rises within weeks of smoking cessation and continues improving over months.
Moderate Alcohol Consumption
Moderate alcohol consumption (particularly red wine) is associated with higher HDL in observational studies. However, the relationship is complex, and alcohol has other health effects that limit recommendations. If you drink moderately already, it may contribute to HDL levels. If you don’t drink, don’t start for HDL benefits alone.
Address Metabolic Health
Insulin resistance and metabolic syndrome suppress HDL. Improving insulin sensitivity through exercise, body composition optimization, and dietary quality often raises HDL substantially as metabolic health improves.
If you have prediabetes or type 2 diabetes, optimizing blood sugar control typically improves lipid profiles including HDL levels.
Optimize Thyroid Function
Hypothyroidism elevates LDL and total cholesterol while potentially lowering HDL. If your thyroid function is suboptimal, addressing it often improves your cholesterol/HDL ratio without other interventions.
Consider Timing and Consistency
Lipid profiles can fluctuate based on recent diet, exercise, stress, and other factors. Consistent healthy habits over months and years produce stable improvements in your ratio. Short-term interventions before testing may create temporary improvements that don’t reflect your true long-term risk.
Cholesterol/HDL Ratio and Other Health Markers
Your cholesterol/HDL ratio doesn’t exist in isolation. Understanding how it relates to other markers provides a more complete cardiovascular risk picture.
Triglycerides
Elevated triglycerides often coincide with low HDL, creating a particularly unfavorable lipid profile. The combination of high triglycerides and low HDL (reflected in a high cholesterol/HDL ratio) indicates metabolic dysfunction and substantially elevated cardiovascular risk.
Interventions that improve one often improve the other. Reducing refined carbohydrates, increasing exercise, and improving body composition typically lower triglycerides while raising HDL.
LDL Cholesterol
LDL cholesterol is the primary component of total cholesterol in most people. High LDL elevates total cholesterol and worsens your ratio. However, the cholesterol/HDL ratio often predicts risk better than LDL alone.
Some people with moderately elevated LDL but excellent HDL (creating a favorable ratio) have lower actual cardiovascular risk than those with “optimal” LDL but very low HDL (creating a poor ratio).
Inflammatory Markers
High-sensitivity C-reactive protein (hs-CRP) and other inflammatory markers often correlate with poor cholesterol/HDL ratios. The combination of unfavorable lipids and elevated inflammation creates particularly high cardiovascular risk.
Addressing inflammation through lifestyle optimization, managing chronic infections or autoimmune conditions, and reducing metabolic dysfunction often improves both inflammatory markers and lipid ratios.
Blood Pressure
Hypertension and poor lipid profiles often occur together, multiplying cardiovascular risk. Optimizing your cholesterol/HDL ratio while managing blood pressure provides synergistic benefits for cardiovascular health.
Insulin and Glucose
Insulin resistance and elevated blood sugar suppress HDL and worsen cholesterol/HDL ratios. Metabolic optimization that improves insulin sensitivity typically improves lipid profiles as a natural consequence.
Cholesterol/HDL Ratio: Frequently Asked Questions
What’s more important: total cholesterol or cholesterol/HDL ratio?
The ratio is far more predictive of cardiovascular risk than total cholesterol alone. You can have elevated total cholesterol with low risk if your HDL is proportionally high, or normal total cholesterol with elevated risk if your HDL is too low. Focus on the ratio rather than obsessing over total cholesterol.
Can I have a good ratio with high total cholesterol?
Yes. If your total cholesterol is 240 mg/dL but your HDL is 80 mg/dL, your ratio is 3.0 (optimal). Many people with moderately elevated total cholesterol have excellent ratios and low actual cardiovascular risk when HDL is high.
Can I have a bad ratio with normal total cholesterol?
Yes. If your total cholesterol is 180 mg/dL but your HDL is only 30 mg/dL, your ratio is 6.0 (high risk). “Normal” total cholesterol provides no protection if HDL is insufficient.
How long does it take to improve my ratio?
HDL responds to lifestyle changes over weeks to months. Consistent exercise often raises HDL noticeably within 6-12 weeks. Body composition changes take longer but produce sustained improvements. Expect to see meaningful ratio improvements within 3-6 months of consistent lifestyle optimization.
Should I take medication to improve my ratio?
Statins lower LDL and total cholesterol but have modest effects on HDL. Fibrates and niacin can raise HDL but have limitations and side effects. For most people, lifestyle optimization should be the primary approach, with medications considered if lifestyle changes are insufficient or if cardiovascular risk is very high.
Does the ratio matter if I’m young?
Yes. Atherosclerosis begins in your 20s and 30s. Optimizing your ratio early prevents decades of arterial damage rather than trying to reverse damage that’s already occurred. Prevention is far more effective than late-stage intervention.
Can I lower my ratio too much?
Extremely low ratios (less than 2.0) typically indicate very high HDL, which is generally considered beneficial. There’s no established “too low” threshold for the ratio itself, though extremely high HDL (above 100 mg/dL) occasionally indicates rare genetic conditions worth investigating.
Testing Cholesterol/HDL Ratio With Apex
Understanding your cholesterol/HDL ratio is essential for cardiovascular optimization and long-term health. This simple metric predicts heart disease risk more accurately than total cholesterol alone, yet many people never calculate or track it.
Our comprehensive blood panel includes complete lipid analysis (total cholesterol, HDL, LDL, triglycerides) alongside 100+ other biomarkers across hormones, metabolism, inflammation, and organ function. This provides complete context for understanding not just your ratio, but the metabolic factors affecting it and the broader implications for your cardiovascular health.
Testing costs $189 with results available in 3-5 business days. Every result is reviewed by licensed medical professionals who provide detailed interpretation focused on optimization, not just disease screening.
If your cholesterol/HDL ratio is elevated, we connect you with medical professionals who understand cardiovascular optimization and can discuss comprehensive strategies for improvement through lifestyle, and when appropriate, targeted interventions.
Get Comprehensive Testing – $189 | Schedule Free Consultation
The Bottom Line on Cholesterol/HDL Ratio
Your cholesterol/HDL ratio matters more for cardiovascular risk than your total cholesterol number. You can have “high” cholesterol with low risk, or “normal” cholesterol with elevated risk, depending on your HDL levels and the resulting ratio.
The standard medical approach focuses primarily on lowering LDL and total cholesterol, often ignoring HDL optimization entirely. The optimization approach recognizes that raising HDL through exercise, body composition improvement, and metabolic health optimization provides powerful cardiovascular protection regardless of where total cholesterol sits.
A ratio below 3.0 indicates excellent cardiovascular health. A ratio above 5.0 indicates elevated risk requiring intervention. Most people fall somewhere in between, with substantial room for improvement through consistent lifestyle optimization.
You can’t optimize what you don’t measure. If you haven’t calculated your cholesterol/HDL ratio and tracked it over time, you’re missing one of the most important predictors of your long-term cardiovascular health.
Stop accepting “normal” when optimal is possible.
Medical Disclaimer: This information is for educational purposes and does not constitute medical advice. Elevated cholesterol/HDL ratios and cardiovascular disease risk require evaluation by qualified healthcare providers. Never make treatment decisions based solely on internet information. Always consult licensed medical professionals for diagnosis and treatment of cardiovascular conditions.
