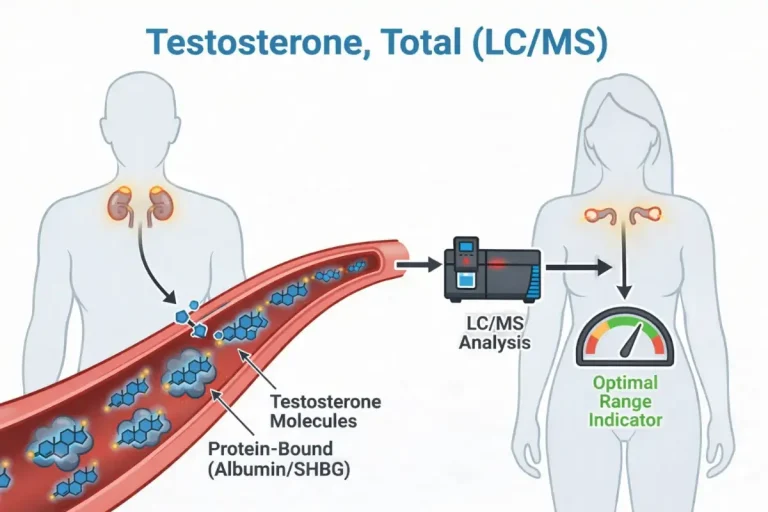
Testosterone, Total (LC/MS): Understanding Your Master Performance Hormone
Testosterone is the primary male sex hormone and one of the most critical biomarkers for energy, strength, mental clarity, and overall vitality in both men and women. Total testosterone measured by LC/MS (liquid chromatography/mass spectrometry) provides the most accurate assessment of your testosterone levels, free from the interference that can affect immunoassay testing.
For high performers, testosterone isn’t just about avoiding deficiency. It’s about optimizing the hormone that drives muscle growth, fat loss, cognitive performance, libido, and competitive drive. Understanding your total testosterone and comparing it to optimal ranges, not just “normal,” is essential for peak performance.
What Is Total Testosterone?
Total testosterone represents the complete amount of testosterone in your blood, including both bound and unbound (free) testosterone. Most testosterone in your body (about 98%) is bound to proteins like sex hormone-binding globulin (SHBG) and albumin, while a small percentage circulates freely and is immediately bioavailable to your tissues.
The LC/MS testing method uses liquid chromatography and mass spectrometry to precisely measure testosterone levels. This is the gold standard for testosterone testing because it’s significantly more accurate than older immunoassay methods, particularly at lower levels. For women and men with low testosterone, LC/MS provides the accuracy needed for proper diagnosis and treatment decisions.
Total testosterone gives you the big picture of your hormonal status. While free testosterone tells you what’s immediately available, total testosterone reflects your overall androgenic capacity and serves as the primary marker for diagnosing low testosterone (hypogonadism) or monitoring testosterone replacement therapy.
Why Total Testosterone Matters for Performance and Health
Testosterone is often called the “master hormone” for good reason. It influences virtually every system in your body that affects performance, body composition, and quality of life.
For men, optimal testosterone drives muscle protein synthesis and strength gains, fat metabolism and lean body composition, bone density and skeletal health, red blood cell production and oxygen delivery, cognitive function including memory and focus, mood regulation and competitive drive, libido and sexual function, and cardiovascular health when properly balanced.
For women, testosterone plays a crucial but often overlooked role in maintaining muscle mass and strength, energy and vitality, libido and sexual satisfaction, bone density, and mental clarity. Women produce testosterone at much lower levels than men, but it’s still essential for optimal health and performance.
Suboptimal testosterone doesn’t just mean you feel tired or have a low sex drive. It means you’re operating below your biological potential across multiple dimensions of performance and health.
Normal vs. Optimal Total Testosterone Levels
Standard Reference Ranges
Men: Most labs report “normal” total testosterone as 264-916 ng/dL, with some variations depending on the lab.
Women: Typical reference ranges are 8-60 ng/dL for adult women, though this varies by age and menopausal status.
The Problem With “Normal”
Here’s the issue with standard reference ranges: they’re based on population averages that include sick, sedentary, and elderly individuals. A 25-year-old athlete being told his 350 ng/dL testosterone is “normal” is being compared to a dataset that includes 80-year-old men with chronic disease.
“Normal for your age” is one of the most frustrating phrases in medicine because it accepts decline as inevitable. Your doctor might see 300 ng/dL in a 40-year-old and call it normal. You’ll feel the difference between 300 and 700 ng/dL every single day.
The bottom of the reference range (264 ng/dL for men) is often where symptomatic hypogonadism begins. You’re technically “normal” but functionally impaired. That’s not a standard any high performer should accept.
Optimal Range for Performance and Longevity
Men: For peak performance, cognitive function, body composition, and quality of life, optimal total testosterone is typically 700-900 ng/dL or higher. Some high-performing men feel best at 800-1000+ ng/dL. Age-related decline is real, but it’s not something you have to accept without intervention.
Women: Optimal ranges for women are less clearly defined in research, but many women report peak energy, libido, and performance with total testosterone in the upper half of the reference range (30-60 ng/dL). Women on hormone replacement therapy sometimes optimize at levels slightly above the standard range under physician supervision.
Optimization isn’t about chasing the highest number possible. It’s about finding the level where you feel energized, recover well, maintain lean mass, have strong libido, and experience mental clarity without negative side effects.
Symptoms of Low Total Testosterone
Low testosterone manifests differently depending on how far below optimal you are, but common symptoms include decreased energy and chronic fatigue, reduced muscle mass and increased body fat (especially abdominal fat), low libido and erectile dysfunction (men) or reduced sexual desire (women), brain fog and poor concentration, decreased motivation and competitive drive, mood changes including irritability and depression, poor recovery from exercise, reduced bone density over time, and sleep disturbances.
In men, symptoms often appear gradually as testosterone declines with age (typically 1-2% per year after age 30). But low testosterone can also affect younger men due to obesity, chronic stress, poor sleep, metabolic dysfunction, or medical conditions.
In women, low testosterone can result from menopause, ovarian dysfunction, adrenal insufficiency, or certain medications. Women often describe feeling like they’ve lost their spark, drive, or vitality when testosterone drops too low.
Symptoms of High Total Testosterone
Excessively high testosterone is less common naturally but can occur with testosterone replacement therapy, anabolic steroid use, or certain medical conditions.
In men, excessively high levels may cause acne and oily skin, increased aggression or irritability, accelerated hair loss (if genetically predisposed), elevated red blood cell count (polycythemia), prostate enlargement (though the link to prostate cancer is not supported by current evidence), and testicular atrophy (when using external testosterone).
In women, high testosterone can indicate polycystic ovary syndrome (PCOS) or other hormonal imbalances and may cause irregular periods, hirsutism (excess facial or body hair), acne, and voice deepening at very high levels.
Optimal testosterone requires balance. More isn’t always better, especially if it comes with side effects or health risks.
What Causes Low Total Testosterone?
Low testosterone can result from a wide range of factors, both lifestyle-related and medical.
Common causes include aging (natural decline after age 30 in men), obesity and metabolic syndrome (fat tissue converts testosterone to estrogen), chronic stress and elevated cortisol, poor sleep quality or sleep apnea, lack of exercise or overtraining, nutrient deficiencies (zinc, vitamin D, magnesium), excessive alcohol consumption, certain medications (opioids, corticosteroids), and medical conditions (hypogonadism, pituitary dysfunction, testicular injury or infection, chronic illness).
For women, causes include menopause and age-related ovarian decline, PCOS and hormonal imbalances, adrenal insufficiency, removal of ovaries (surgical menopause), and certain medications (oral contraceptives, corticosteroids).
In many cases, low testosterone is multifactorial. A sedentary 45-year-old man who’s overweight, sleeps poorly, and drinks heavily isn’t just dealing with age-related decline. He’s experiencing the compounding effects of multiple risk factors.
What Causes High Total Testosterone?
Naturally high testosterone within healthy ranges is generally not a concern and may simply reflect good genetics, youth, and healthy lifestyle factors.
Abnormally high testosterone can result from testosterone replacement therapy or anabolic steroid use, polycystic ovary syndrome (PCOS) in women, adrenal tumors or disorders, and testicular tumors (rare).
If your testosterone is significantly above the reference range and you’re not on replacement therapy, medical evaluation is warranted to rule out underlying conditions.
How to Optimize Total Testosterone
Lifestyle Interventions
Before considering medical interventions, optimize the foundational factors that support healthy testosterone production.
Strength Training: Heavy resistance training, particularly compound movements like squats, deadlifts, and presses, stimulates testosterone production. Training to near failure with adequate rest between sets is most effective.
Sleep Optimization: Testosterone is primarily produced during sleep. Poor sleep quality or insufficient sleep (less than 7 hours) significantly lowers testosterone. Sleep apnea is a major contributor to low T and should be evaluated and treated.
Body Composition: Losing excess body fat, especially visceral fat, can significantly improve testosterone levels. Fat tissue contains aromatase, an enzyme that converts testosterone to estrogen. Reducing body fat reduces this conversion.
Stress Management: Chronic stress elevates cortisol, which suppresses testosterone production. Mindfulness, adequate downtime, and managing life stressors all support hormonal balance.
Nutrition: Adequate protein, healthy fats (especially saturated and monounsaturated fats), and micronutrients like zinc, magnesium, and vitamin D support testosterone production. Severe calorie restriction or very low-fat diets can tank testosterone.
Limit Alcohol: Excessive alcohol consumption directly suppresses testosterone production and increases estrogen. Moderate intake is fine, but chronic heavy drinking is one of the fastest ways to crash your testosterone.
Avoid Overtraining: While exercise boosts testosterone, chronic overtraining without adequate recovery raises cortisol and lowers testosterone. Balance intensity with rest.
Medical Interventions
When lifestyle optimization isn’t enough, or when testosterone levels are clinically low, medical interventions can restore levels to optimal ranges.
Testosterone Replacement Therapy (TRT): For men with diagnosed low testosterone, TRT is the most direct and effective intervention. Options include injectable testosterone (most common and effective), topical testosterone creams or gels, and testosterone pellets (implanted under the skin). TRT is a long-term commitment and requires ongoing medical monitoring. Learn more about ApexBlood’s TRT program.
Enclomiphene: For younger men or those concerned about fertility, enclomiphene stimulates natural testosterone production by blocking estrogen receptors in the pituitary gland. This increases luteinizing hormone (LH) and follicle-stimulating hormone (FSH), which signal the testes to produce more testosterone. It’s an alternative to TRT for some patients.
Hormone Replacement Therapy (HRT) for Women: Women experiencing low testosterone due to menopause or other hormonal imbalances may benefit from testosterone as part of a comprehensive hormone replacement strategy. This is typically combined with estrogen and progesterone depending on individual needs. Learn more about ApexBlood’s HRT program.
Addressing Underlying Conditions: If low testosterone is caused by sleep apnea, pituitary dysfunction, or other medical conditions, treating the root cause may restore normal levels without direct testosterone supplementation.
Medical interventions should always be supervised by a qualified physician who monitors your levels, manages side effects, and adjusts treatment based on your individual response.
Total Testosterone and Other Health Markers
Testosterone doesn’t exist in isolation. It interacts with multiple other biomarkers and hormones that influence how you feel and perform.
Free Testosterone: While total testosterone tells you the overall amount, free testosterone (the unbound, bioavailable form) is what actually drives tissue effects. Some men have normal total testosterone but low free testosterone due to high SHBG. Both markers should be evaluated together.
Sex Hormone-Binding Globulin (SHBG): SHBG binds testosterone and reduces the amount of free testosterone available to tissues. High SHBG (often caused by aging, hyperthyroidism, or low insulin) can cause symptoms of low testosterone even when total levels are normal. Low SHBG (often seen with obesity, insulin resistance, or hypothyroidism) increases free testosterone but may indicate metabolic dysfunction.
Estradiol: Testosterone is converted to estradiol (a form of estrogen) by the aromatase enzyme, especially in fat tissue. Men need some estradiol for bone health, libido, and cardiovascular function, but excessively high estradiol can cause gynecomastia (breast tissue growth), water retention, and mood issues. Monitoring estradiol is essential during TRT.
Luteinizing Hormone (LH) and Follicle-Stimulating Hormone (FSH): These pituitary hormones signal the testes (in men) or ovaries (in women) to produce testosterone. Low testosterone with low LH/FSH suggests pituitary dysfunction (secondary hypogonadism). Low testosterone with high LH/FSH suggests testicular or ovarian failure (primary hypogonadism).
Hemoglobin and Hematocrit: Testosterone stimulates red blood cell production. Men on TRT may experience elevated hemoglobin and hematocrit, which increases oxygen-carrying capacity but can also increase blood viscosity and cardiovascular risk if too high. Monitoring complete blood count (CBC) is essential during TRT.
Prostate-Specific Antigen (PSA): While modern research has debunked the myth that testosterone causes prostate cancer, PSA is still monitored during TRT to screen for prostate issues. Rapidly rising PSA warrants further evaluation.
Thyroid Hormones: Hypothyroidism can lower testosterone by increasing SHBG and reducing free testosterone. Optimizing thyroid function (TSH, free T3, free T4) often improves testosterone levels and symptoms.
Cortisol: Chronic stress and elevated cortisol suppress testosterone production. Optimizing both hormones simultaneously is often necessary for peak performance.
Insulin and Glucose: Insulin resistance and metabolic syndrome lower testosterone. Improving insulin sensitivity through diet, exercise, and weight loss often raises testosterone levels naturally.
Total Testosterone and Hormone Optimization
Optimizing testosterone is rarely about testosterone alone. It’s about balancing the entire hormonal system to support energy, performance, body composition, and longevity.
For men, this often means TRT or natural optimization strategies combined with attention to thyroid function, cortisol management, and metabolic health. Estradiol management may be necessary for some men on TRT, though blanket use of aromatase inhibitors is not recommended without clinical justification.
For women, testosterone optimization is typically part of a broader hormone replacement strategy that includes estrogen and progesterone. Perimenopause and menopause dramatically alter the hormonal landscape, and addressing testosterone alongside other hormones can restore energy, libido, and quality of life.
Whether you’re a man dealing with age-related decline or a woman navigating hormonal changes, comprehensive blood testing provides the data you need to make informed decisions. ApexBlood’s testing includes testosterone alongside 100+ other biomarkers, giving you the complete picture of your hormonal health.
Frequently Asked Questions
What’s the difference between total testosterone and free testosterone?
Total testosterone measures all the testosterone in your blood, including testosterone bound to proteins like SHBG and albumin. Free testosterone measures only the unbound testosterone that’s immediately available to your tissues. Both markers are important. Some people have normal total testosterone but low free testosterone due to high SHBG, which can still cause symptoms of low T.
Why is LC/MS testing better than immunoassay testing?
LC/MS (liquid chromatography/mass spectrometry) is significantly more accurate than older immunoassay methods, particularly at lower testosterone levels. Immunoassays can be affected by cross-reactivity with other molecules, leading to falsely high or low readings. LC/MS is the gold standard for testosterone testing, especially for women and men with low testosterone.
Can lifestyle changes really increase testosterone?
Yes, but the degree of increase depends on the cause of low testosterone. If your levels are low due to obesity, poor sleep, or chronic stress, lifestyle interventions can produce meaningful improvements (often 100-200 ng/dL or more). However, if you have primary or secondary hypogonadism, lifestyle changes alone are unlikely to restore optimal levels. Medical intervention may be necessary.
At what level should I consider testosterone replacement therapy?
There’s no universal cutoff. Some men feel terrible at 400 ng/dL, while others feel fine. Clinical guidelines often use 300 ng/dL as a threshold for hypogonadism, but symptoms matter more than numbers. If you’re experiencing symptoms of low testosterone and your levels are below 500-600 ng/dL, TRT may be worth discussing with a physician. Many men report feeling best at 700-900 ng/dL or higher.
Can women take testosterone?
Yes. Women produce testosterone naturally, and it plays an important role in energy, libido, muscle mass, and overall vitality. Testosterone is sometimes prescribed as part of hormone replacement therapy for women experiencing menopause or other hormonal imbalances. Dosing is much lower for women than men, and treatment must be carefully monitored.
Does testosterone replacement therapy cause prostate cancer?
No. This myth has been thoroughly debunked by modern research. Testosterone does not cause prostate cancer. Men on TRT are still monitored for prostate health (via PSA testing and digital rectal exams), but there’s no evidence that TRT increases prostate cancer risk in men without pre-existing cancer.
Will my natural testosterone production shut down on TRT?
Yes. When you take external testosterone, your body stops producing its own because the feedback loop signals that you have sufficient testosterone. This is why TRT is typically a long-term commitment. Some men use enclomiphene or HCG to maintain natural production, but these approaches are less effective than TRT for raising levels.
How often should I test my testosterone?
If you’re not on TRT or experiencing symptoms, annual testing is reasonable to track trends. If you’re optimizing lifestyle factors, retesting every 3-6 months can help you see whether interventions are working. If you’re on TRT, testing every 3-6 months during dose titration and then annually once stable is standard. Your physician may recommend more frequent monitoring if adjustments are needed.
What time of day should I test testosterone?
Testosterone levels are highest in the morning (typically 8-10 AM) and decline throughout the day. For accurate and consistent results, always test in the morning. If you’re on TRT, your physician may request testing at specific times relative to your injection schedule to assess peak and trough levels.
Can stress really lower testosterone that much?
Yes. Chronic stress elevates cortisol, which directly suppresses testosterone production. Men experiencing prolonged stress (work, relationships, financial pressure) often see significant drops in testosterone. Managing stress through sleep, downtime, and lifestyle adjustments can restore levels in some cases.
Is it normal for testosterone to decline with age?
Yes, testosterone typically declines by about 1-2% per year after age 30 in men. This is “normal” in the sense that it’s common, but it’s not something you have to accept. Many men maintain high testosterone well into their 60s and beyond through lifestyle optimization or TRT. “Normal for your age” is a medical cop-out when optimal is possible.
What if my testosterone is normal but I still feel terrible?
Look at free testosterone, SHBG, thyroid hormones, cortisol, and other markers. Sometimes total testosterone is “normal” but free testosterone is low due to high SHBG. Other times, the issue isn’t testosterone at all but thyroid dysfunction, adrenal fatigue, insulin resistance, or nutrient deficiencies. Comprehensive blood testing provides the full picture.
Testing Total Testosterone With ApexBlood
Total testosterone (LC/MS) is included in ApexBlood’s comprehensive blood panel alongside 100+ other biomarkers. We don’t just test testosterone in isolation. We measure free testosterone, SHBG, estradiol, thyroid hormones, metabolic markers, and more to give you the complete context you need to optimize your hormones and performance.
Our testing uses LC/MS for maximum accuracy, and you’ll receive results with clear explanations of what they mean for your health and performance. If your levels are suboptimal, you’ll have direct access to physician consultations and treatments like TRT or HRT to bring your hormones back to optimal ranges.
Get comprehensive testing for $189 and see where you stand.
The Bottom Line on Total Testosterone
Testosterone is one of the most important biomarkers for energy, performance, body composition, mental clarity, and quality of life. Whether you’re a man experiencing age-related decline or a woman navigating hormonal changes, optimizing testosterone can dramatically improve how you feel and perform.
Standard reference ranges tell you what’s “normal” for a population that includes sick, sedentary, and elderly individuals. Optimal ranges tell you what’s possible when you refuse to settle for average. The difference between 350 ng/dL and 800 ng/dL is the difference between struggling through your day and dominating it.
You can’t optimize what you don’t measure. Comprehensive blood testing gives you the data you need to understand your testosterone levels, identify what’s holding you back, and take action to restore your hormones to optimal ranges.
Stop accepting “normal for your age” when optimal is possible.
Medical Disclaimer: This information is for educational purposes and does not constitute medical advice. Testosterone levels and hormone optimization require evaluation by qualified healthcare providers. Never make treatment decisions based solely on internet information. Always consult licensed medical professionals for diagnosis and treatment.
