Hemoglobin: The Oxygen Transport System That Powers Performance
You’re exhausted during workouts that used to feel manageable. Your mental clarity isn’t what it was. You’re cold when others are comfortable. Your doctor runs a complete blood count and finds your hemoglobin is 12.5 g/dL—technically “normal” but nowhere near optimal.
Meanwhile, high-performing athletes maintain hemoglobin between 15-17 g/dL, ensuring maximum oxygen delivery to tissues, optimal energy production, and peak physical and cognitive performance.
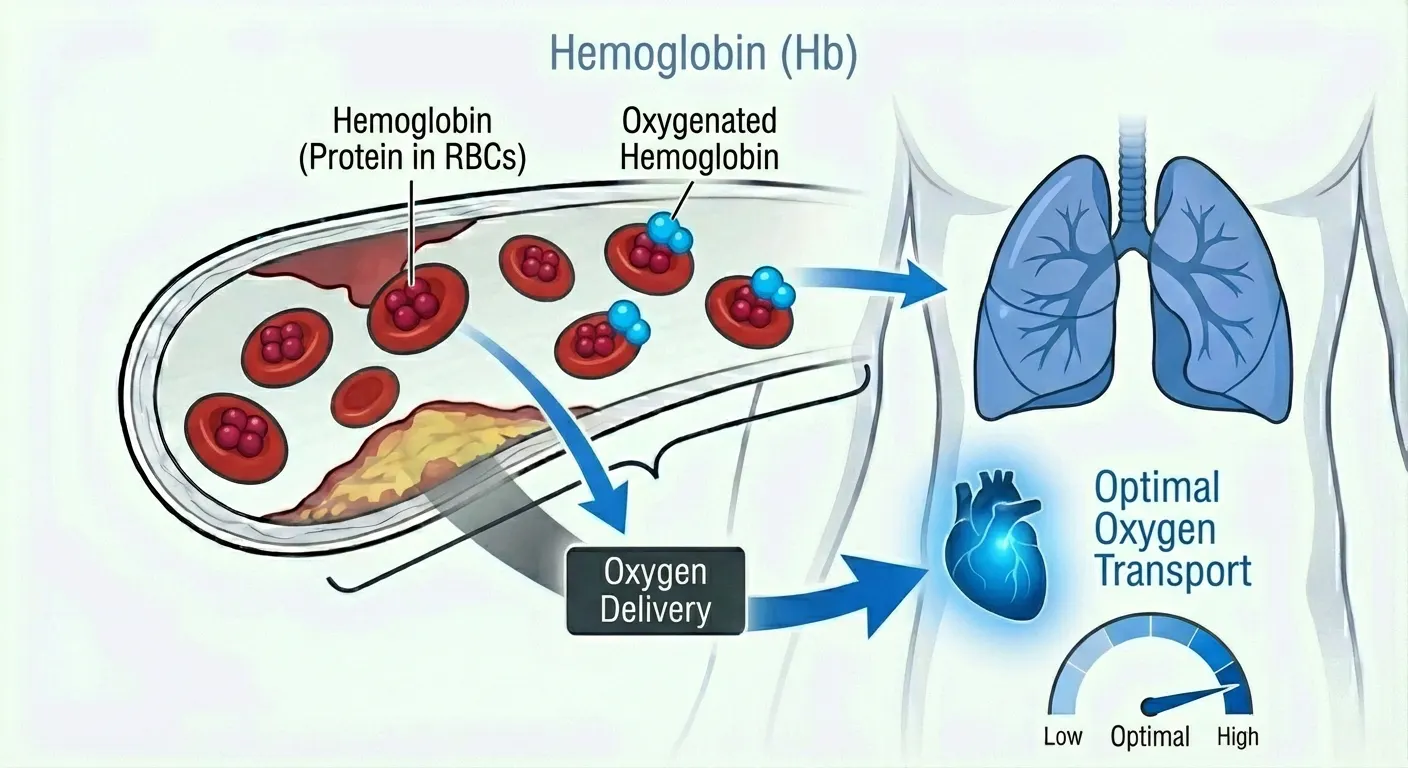
Hemoglobin is the protein inside red blood cells that carries oxygen from your lungs to every cell in your body and returns carbon dioxide to your lungs for exhalation. It’s not just about preventing anemia—it’s about optimizing the oxygen delivery system that powers everything from ATP production in your mitochondria to cognitive function in your brain.
Low-normal hemoglobin means you’re operating below your biological potential. Your cells aren’t getting optimal oxygen. Your mitochondria can’t produce energy efficiently. Your physical and mental performance suffers even when you’re not technically “anemic.”
High performers don’t accept “within normal range” when normal includes sedentary, unhealthy populations. They optimize hemoglobin for peak oxygen delivery and maximum cellular energy production.
What Is Hemoglobin?
Hemoglobin is an iron-containing protein found inside red blood cells (erythrocytes). Each red blood cell contains approximately 270 million hemoglobin molecules, and each hemoglobin molecule can bind four oxygen molecules.
This oxygen-carrying capacity is what makes hemoglobin critical for life. Your tissues require constant oxygen delivery for cellular respiration—the process by which mitochondria convert glucose and oxygen into ATP (adenosine triphosphate), the energy currency that powers every cellular process in your body.
Hemoglobin structure consists of four protein subunits (two alpha chains and two beta chains), each containing a heme group. The heme group contains iron, which directly binds oxygen. When oxygen binds to hemoglobin in the lungs, it forms oxyhemoglobin (bright red). When oxygen is released to tissues, it forms deoxyhemoglobin (darker red).
The oxygen binding and release process is remarkably sophisticated. Hemoglobin has high affinity for oxygen in the lungs (where oxygen concentration is high) and lower affinity in tissues (where oxygen concentration is low and carbon dioxide concentration is high). This allows efficient oxygen pickup in the lungs and efficient oxygen delivery where it’s needed.
Hemoglobin also transports carbon dioxide (about 20-25% of total CO2 transport) from tissues back to the lungs, though most carbon dioxide is transported dissolved in plasma or as bicarbonate ions.
Your body produces approximately 2 million new red blood cells every second to replace those that die (red blood cells live about 120 days). This constant production requires adequate iron, vitamin B12, folate, protein, and other nutrients. Hemoglobin synthesis occurs primarily in developing red blood cells in the bone marrow.
Why Hemoglobin Matters for Performance and Health
Hemoglobin determines your oxygen-carrying capacity—the amount of oxygen your blood can deliver to tissues with each heartbeat. This directly impacts every system in your body.
Physical performance depends on oxygen delivery to muscles. During exercise, muscles consume oxygen at dramatically higher rates to produce ATP for contraction. Higher hemoglobin means more oxygen delivery per unit of blood, allowing greater exercise capacity, better endurance, faster recovery between efforts, and reduced fatigue. Athletes with optimized hemoglobin can sustain higher power outputs and maintain intensity longer than those with low-normal hemoglobin.
This is why altitude training works—exposure to low oxygen at altitude stimulates increased red blood cell and hemoglobin production, improving oxygen-carrying capacity when athletes return to sea level. It’s also why EPO (erythropoietin) doping is so effective and heavily banned in sports—artificially increasing hemoglobin provides enormous performance advantages.
Cognitive function requires massive oxygen delivery to the brain. Your brain represents about 2% of body weight but consumes 20% of your oxygen supply. Hemoglobin directly determines how much oxygen reaches brain tissue. Low or low-normal hemoglobin impairs cognitive function through reduced mental clarity and processing speed, increased brain fog and difficulty concentrating, impaired memory formation and recall, and reduced executive function and decision-making capacity.
Many people operating with hemoglobin in the low-normal range (11-13 g/dL) experience chronic cognitive symptoms they attribute to stress, aging, or poor sleep when the underlying issue is insufficient oxygen delivery to the brain.
Energy production and fatigue are directly linked to oxygen availability. ATP production through aerobic metabolism (in mitochondria) requires oxygen. When oxygen delivery is suboptimal due to low hemoglobin, cells must rely more heavily on anaerobic metabolism, which produces far less ATP and generates lactate. The result is chronic fatigue, reduced stamina throughout the day, feeling exhausted by activities that should be manageable, and longer recovery times after exertion.
This isn’t clinical anemia requiring medical intervention—it’s suboptimal oxygen delivery impairing daily function and performance.
Cold tolerance depends partly on oxygen availability for heat production. People with low or low-normal hemoglobin often feel cold when others are comfortable because their tissues aren’t receiving optimal oxygen for metabolic heat generation.
Immune function requires adequate oxygen for white blood cell activity. Hemoglobin indirectly supports immune responses by ensuring immune cells receive the oxygen needed for their high metabolic demands during infection fighting.
Wound healing and tissue repair require oxygen for collagen synthesis, cell proliferation, and tissue remodeling. Low hemoglobin slows recovery from injuries and surgical procedures.
Normal vs. Optimal Hemoglobin Levels
Standard reference ranges for hemoglobin vary slightly by laboratory but typically show:
Men: 13.5-17.5 g/dL
Women: 12.0-15.5 g/dL
Anemia is typically diagnosed when hemoglobin falls below 13.0 g/dL in men or 12.0 g/dL in women.
The problem with these ranges is they include sedentary, unhealthy individuals with suboptimal nutrition, chronic disease, and poor metabolic health. “Normal for the population” is not the same as “optimal for performance.”
Optimal hemoglobin for performance and vitality:
Men: 15.0-17.0 g/dL, ideally 15.5-16.5 g/dL
Women: 14.0-16.0 g/dL, ideally 14.5-15.5 g/dL
These targets reflect the hemoglobin levels seen in healthy, active individuals with excellent nutrition and optimal iron status. Athletes often maintain hemoglobin at the higher end of reference ranges or even slightly above.
The difference between low-normal and optimal hemoglobin is substantial. A man with hemoglobin at 13.5 g/dL (low-normal) versus 16.0 g/dL (optimal) has approximately 18% less oxygen-carrying capacity. Over time, this difference dramatically impacts energy, performance, recovery, and cognitive function.
For women, the distinction is equally important. A woman with hemoglobin at 12.5 g/dL (low-normal) versus 15.0 g/dL (optimal) has about 20% less oxygen-carrying capacity. Many women operate chronically in the low-normal range due to menstrual blood loss and inadequate iron intake, accepting fatigue and reduced performance as normal when they’re actually experiencing suboptimal oxygen delivery.
Important caveat: Very high hemoglobin (above 18-19 g/dL in men, above 16-17 g/dL in women) can indicate polycythemia—abnormally elevated red blood cell production that increases blood viscosity and cardiovascular risk. Extremely high hemoglobin requires medical evaluation.
What Causes Low Hemoglobin?
Understanding what drives low hemoglobin reveals what you need to optimize.
Iron deficiency is the most common cause of low hemoglobin globally. Iron is required for heme synthesis—without adequate iron, you can’t produce functional hemoglobin. Iron deficiency develops through inadequate dietary intake (particularly in people avoiding red meat), poor iron absorption (celiac disease, inflammatory bowel disease, H. pylori infection, low stomach acid), blood loss (menstruation, gastrointestinal bleeding, frequent blood donation), and increased iron demands (pregnancy, rapid growth, intense training).
Iron deficiency anemia develops progressively: first, iron stores (ferritin) deplete; then, iron available for hemoglobin production declines; finally, hemoglobin production falls and anemia develops. Many people experience symptoms when ferritin is low even before hemoglobin declines significantly.
Vitamin B12 and folate deficiencies impair red blood cell production. These vitamins are essential for DNA synthesis in rapidly dividing cells like red blood cell precursors in bone marrow. Deficiency causes megaloblastic anemia—production of abnormally large, dysfunctional red blood cells and reduced overall red blood cell count. B12 deficiency occurs from inadequate intake (strict vegan diets without supplementation), poor absorption (pernicious anemia, gastric surgery, low stomach acid), or certain medications (metformin, PPIs). Folate deficiency occurs from inadequate intake, poor absorption, or increased demands (pregnancy).
Chronic inflammation suppresses hemoglobin production. Inflammatory cytokines impair iron utilization, reduce erythropoietin (EPO) production (the hormone that stimulates red blood cell production), and shorten red blood cell lifespan. This creates “anemia of chronic disease”—hemoglobin drops despite adequate iron stores. Common causes include autoimmune conditions, chronic infections, inflammatory bowel disease, and obesity-related chronic inflammation.
Kidney disease reduces erythropoietin production. The kidneys produce EPO in response to low oxygen levels. When kidney function declines, EPO production falls, leading to reduced red blood cell and hemoglobin production. This is why chronic kidney disease commonly causes anemia.
Blood loss from any source reduces hemoglobin. Menstruation is a major cause in women—monthly blood loss of 30-80 mL depletes iron stores and reduces hemoglobin over time without adequate iron repletion. Gastrointestinal bleeding from ulcers, gastritis, inflammatory bowel disease, or colon polyps/cancer causes chronic blood loss that may not be obvious. Frequent blood donation (more than 2-3 times per year) can deplete iron stores and reduce hemoglobin.
Genetic conditions affecting hemoglobin production include thalassemia (genetic defects in hemoglobin chain production), sickle cell trait or disease (abnormal hemoglobin structure), and other hemoglobinopathies. These conditions are relatively common in certain populations and require specific management.
Bone marrow disorders impair red blood cell production including aplastic anemia, myelodysplastic syndromes, leukemia, and bone marrow infiltration by other diseases.
Medications can reduce hemoglobin including chemotherapy drugs that suppress bone marrow, certain antibiotics, anti-inflammatory medications, and medications affecting folate or B12 metabolism.
Hemolysis—premature destruction of red blood cells—reduces hemoglobin through autoimmune hemolytic anemia, inherited conditions like G6PD deficiency, mechanical destruction from heart valve problems or strenuous exercise, or infections.
What Causes High Hemoglobin?
Elevated hemoglobin (above 17.5-18 g/dL in men, above 15.5-16 g/dL in women) requires attention because it can indicate underlying disease or create health risks.
Chronic hypoxia (low oxygen) stimulates increased red blood cell production. Living at high altitude naturally increases hemoglobin—the body compensates for lower oxygen availability by producing more oxygen-carrying capacity. Chronic lung disease (COPD, pulmonary fibrosis) causes chronically low blood oxygen, triggering increased hemoglobin production. Sleep apnea creates intermittent hypoxia that can elevate hemoglobin. Heavy smoking reduces oxygen-carrying capacity of existing hemoglobin, stimulating production of more red blood cells.
Polycythemia vera is a bone marrow disorder causing uncontrolled red blood cell overproduction. This genetic mutation in blood-forming cells leads to progressively increasing hemoglobin, hematocrit, and red blood cell count. Hemoglobin can rise above 18-20 g/dL, increasing blood viscosity and substantially raising risk of blood clots, stroke, and heart attack. This condition requires medical treatment.
Dehydration artificially elevates hemoglobin by concentrating blood. If you’re significantly dehydrated when blood is drawn, hemoglobin appears high because plasma volume is reduced while red blood cell mass remains constant. Rehydration normalizes the measurement. This is why hydration status matters when interpreting hemoglobin.
Testosterone and anabolic steroid use stimulate red blood cell production. Testosterone therapy commonly increases hemoglobin by 0.5-1.5 g/dL or more. While modest increases improve energy and performance, excessive increases (hemoglobin above 18 g/dL) increase cardiovascular risk and may require dose adjustment or therapeutic phlebotomy. Anabolic steroid abuse can cause dangerous hemoglobin elevation.
Secondary polycythemia from other causes includes kidney tumors producing excess EPO, other tumors producing EPO-like substances, and genetic conditions affecting oxygen sensing.
Hemoglobin and Related Blood Markers
Hemoglobin exists within a system of related markers that provide complete context for oxygen-carrying capacity and red blood cell health.
Hematocrit is the percentage of blood volume occupied by red blood cells. Normal ranges are approximately 38-50% for men, 36-44% for women. Hematocrit and hemoglobin move together—low hemoglobin correlates with low hematocrit, high hemoglobin correlates with high hematocrit. The relationship between them reveals red blood cell characteristics.
Red blood cell count (RBC) tells you how many red blood cells you have per microliter of blood. Normal ranges are approximately 4.5-5.9 million/μL for men, 4.1-5.1 million/μL for women. You can have normal RBC count with low hemoglobin if each cell contains less hemoglobin than optimal (hypochromic anemia). You can have low RBC count with normal hemoglobin if each cell contains more hemoglobin than normal (macrocytic conditions).
MCV (mean corpuscular volume) measures the average size of red blood cells. Normal range is approximately 80-100 fL. Low MCV (microcytic anemia) suggests iron deficiency or thalassemia—cells are smaller than normal. High MCV (macrocytic anemia) suggests B12 or folate deficiency, or certain medications—cells are larger than normal. Normal MCV with low hemoglobin suggests chronic disease, recent blood loss, or mixed deficiencies.
MCH (mean corpuscular hemoglobin) measures the average amount of hemoglobin per red blood cell. MCHC (mean corpuscular hemoglobin concentration) measures the concentration of hemoglobin within red blood cells. These markers help classify anemia types and identify specific deficiencies.
RDW (red cell distribution width) measures variation in red blood cell size. High RDW indicates significant variation (some cells much larger or smaller than others), suggesting mixed deficiencies, recent blood loss with new cell production, or certain anemia types.
Ferritin measures iron storage and is critical for understanding iron status. Low ferritin (below 30-50 ng/mL) indicates depleted iron stores even when hemoglobin is still normal. Optimal ferritin for performance is 50-100 ng/mL or higher. Very high ferritin (above 300-400 ng/mL) can indicate iron overload, chronic inflammation, or liver disease.
Iron and TIBC (total iron binding capacity) assess current iron availability. Low iron with high TIBC suggests iron deficiency. Low iron with low TIBC suggests chronic disease. Iron saturation (percentage of TIBC occupied by iron) should be 20-45% for optimal hemoglobin production.
Vitamin B12 should be above 400-500 pg/mL for optimal red blood cell production and neurological function, though standard “normal” starts at 200-300 pg/mL.
Reticulocyte count measures newly produced red blood cells and reveals whether bone marrow is responding appropriately to low hemoglobin. High reticulocytes with low hemoglobin suggest active blood loss or hemolysis (destruction). Low reticulocytes with low hemoglobin suggest impaired production from nutritional deficiency, bone marrow problems, or chronic disease.
How to Optimize Hemoglobin
Optimizing hemoglobin requires ensuring adequate nutrition for red blood cell production and addressing any factors impairing production or increasing loss.
Optimize iron intake and absorption. Consume adequate dietary iron from heme iron sources (red meat, organ meats, shellfish)—most bioavailable form, or non-heme iron sources (legumes, fortified grains, dark leafy greens) with vitamin C to enhance absorption. For people with documented iron deficiency or suboptimal ferritin, iron supplementation may be necessary—typical doses are 25-65 mg elemental iron daily, taken with vitamin C and away from calcium, coffee, or tea which impair absorption. Monitor ferritin to ensure repletion without overload. Target ferritin 50-100 ng/mL or higher for optimal hemoglobin production.
Ensure adequate vitamin B12 intake. Consume B12 from animal products (meat, fish, eggs, dairy)—B12 is not naturally present in plant foods. Vegans and vegetarians require B12 supplementation (at least 250-500 mcg daily) or fortified foods. People with absorption issues (gastric surgery, pernicious anemia, chronic PPI use) may need high-dose oral B12 (1000+ mcg daily) or B12 injections. Optimal B12 is above 400-500 pg/mL.
Include adequate folate from leafy greens, legumes, fortified grains, and citrus fruits. Folate requirements increase during pregnancy. Supplementation (400-800 mcg daily) ensures adequate intake, particularly for people with increased needs or poor dietary intake.
Consume adequate protein for hemoglobin synthesis. Hemoglobin is a protein requiring amino acids for production. Inadequate protein intake impairs red blood cell production. Target at least 0.8-1.0 g/kg body weight minimum, more for athletes and active individuals (1.2-2.0 g/kg).
Address any sources of chronic blood loss. For women with heavy menstrual bleeding, discuss management options with a gynecologist—reducing blood loss preserves iron and hemoglobin. For anyone with suspected gastrointestinal bleeding (black stools, positive occult blood test, unexplained iron deficiency), gastroenterology evaluation is essential. Limit blood donation frequency if you struggle to maintain hemoglobin and ferritin—consider donating no more than 2-3 times yearly and monitor markers regularly.
Reduce chronic inflammation if present. Inflammatory conditions impair hemoglobin production even when iron stores are adequate. Address underlying inflammatory conditions (autoimmune disease, chronic infections, inflammatory bowel disease). Reduce obesity-related inflammation through weight loss. Optimize diet to reduce inflammatory foods. Check hs-CRP to assess systemic inflammation—target below 1.0 mg/L, ideally below 0.5 mg/L.
Ensure adequate hydration for accurate measurement. Dehydration artificially elevates hemoglobin by concentrating blood. For consistent, accurate hemoglobin assessment, be well-hydrated when blood is drawn.
Consider altitude training or hypoxic training for athletes seeking performance gains. Exposure to altitude or hypoxic conditions stimulates EPO production and increases hemoglobin naturally. This requires careful implementation and monitoring to avoid excessive elevation.
Hemoglobin and Performance Enhancement
Athletes and high performers have long understood that hemoglobin directly determines oxygen-carrying capacity and performance. This is why blood doping and EPO use are so heavily regulated in competitive sports—artificially increasing hemoglobin provides enormous advantages.
Legitimate optimization strategies for increasing hemoglobin include ensuring iron stores are optimal (ferritin 50-100+ ng/mL), maintaining excellent B12 and folate status, consuming adequate protein and overall nutrition, altitude training or living at altitude (stimulates natural EPO production), hypoxic training devices (simulate altitude), and for men, optimizing testosterone within physiological ranges (testosterone naturally stimulates red blood cell production).
The difference between optimized hemoglobin and low-normal hemoglobin is dramatic for performance. An athlete with hemoglobin at 16.5 g/dL versus 14.0 g/dL has approximately 18% more oxygen-carrying capacity. In endurance sports, this translates to measurably better performance—higher VO2 max, better lactate threshold, improved time trial performance, and faster recovery.
But benefits extend beyond elite athletics. Anyone engaged in regular exercise, physically demanding work, or seeking optimal energy and cognitive function benefits from optimized hemoglobin. The person with hemoglobin at 15.5 g/dL feels noticeably more energetic, recovers faster from workouts, maintains better focus throughout the day, and tolerates physical demands better than when operating at 13.0 g/dL.
Important distinction: Optimizing hemoglobin through nutrition, iron repletion, and natural EPO stimulation is fundamentally different from pharmacological EPO use or blood doping, which can raise hemoglobin to dangerous levels (above 18-19 g/dL). Extremely high hemoglobin increases blood viscosity and cardiovascular risk. The goal is optimization within healthy ranges, not supraphysiological elevation.
When Low Hemoglobin Requires Medical Attention
While this article focuses on optimization, certain situations require medical evaluation rather than self-directed optimization.
Seek medical evaluation if hemoglobin falls below 12.0 g/dL in men or 11.0 g/dL in women—this represents significant anemia requiring investigation. You have symptoms of severe anemia including severe fatigue or weakness, shortness of breath at rest or with minimal exertion, rapid heartbeat or palpitations, dizziness or lightheadedness, or chest pain. Hemoglobin is dropping progressively despite intervention. You have evidence of bleeding including black or bloody stools, heavy menstrual bleeding, or unexplained bruising. You have other concerning symptoms including unintended weight loss, night sweats, enlarged lymph nodes, bone pain, or other systemic symptoms suggesting underlying disease.
Anemia can be the first sign of serious conditions including gastrointestinal cancers, bone marrow disorders, autoimmune diseases, kidney disease, or other systemic illnesses. Persistent or severe anemia always warrants thorough medical investigation.
Frequently Asked Questions
What is a good hemoglobin level?
For men, optimal is 15.0-17.0 g/dL, ideally 15.5-16.5 g/dL. For women, optimal is 14.0-16.0 g/dL, ideally 14.5-15.5 g/dL. These levels ensure excellent oxygen-carrying capacity for physical performance, cognitive function, and energy production. Standard “normal” ranges include unhealthy populations and don’t represent optimal performance.
Can low hemoglobin cause fatigue even if it’s not anemia?
Yes, absolutely. Hemoglobin at 12.5-13.5 g/dL might be “within normal range” but represents suboptimal oxygen delivery. Many people operating in the low-normal range experience chronic fatigue, reduced exercise capacity, brain fog, and cold intolerance that improve dramatically when hemoglobin is optimized to 15-16 g/dL. You don’t need to be anemic to experience symptoms from suboptimal oxygen-carrying capacity.
How quickly can I increase my hemoglobin?
With adequate iron supplementation and nutrition, hemoglobin typically increases 0.5-1.0 g/dL every 2-3 weeks if iron deficiency was the primary cause. Full optimization might take 2-3 months. Ferritin (iron stores) takes longer to replete—often 3-6 months of supplementation. B12 and folate deficiency anemia responds to supplementation within weeks to months. The timeline depends on the underlying cause and severity of deficiency.
Should I take iron supplements if my hemoglobin is low-normal?
Check ferritin first. If ferritin is below 30-50 ng/mL, you likely have depleted iron stores limiting hemoglobin production, and supplementation is appropriate. If ferritin is adequate (above 50-100 ng/mL) but hemoglobin remains low, investigate other causes—B12 deficiency, folate deficiency, chronic inflammation, or underlying medical conditions. Don’t supplement iron without knowing your iron status—excess iron can be harmful.
Can high hemoglobin be dangerous?
Yes, when hemoglobin rises above 18-19 g/dL in men or 16-17 g/dL in women, blood viscosity increases substantially, raising risk of blood clots, stroke, and heart attack. Very high hemoglobin requires medical evaluation to identify the cause—polycythemia vera, chronic hypoxia, excessive testosterone, or other conditions. Modest elevation (16-17 g/dL in men, 15-16 g/dL in women) is generally not dangerous and often reflects optimal oxygen-carrying capacity.
Does living at altitude increase hemoglobin?
Yes, altitude exposure stimulates EPO production, which increases red blood cell and hemoglobin production. The body compensates for lower oxygen availability at altitude by producing more oxygen-carrying capacity. This adaptation takes 2-4 weeks of altitude exposure and reverses gradually after returning to sea level. Athletes use altitude training specifically to increase hemoglobin and improve performance.
Why do women typically have lower hemoglobin than men?
Several reasons: testosterone stimulates red blood cell production (men have higher testosterone), menstrual blood loss depletes iron stores and reduces hemoglobin over time without adequate repletion, women typically have lower muscle mass and lower metabolic oxygen demands, and evolutionary adaptation to pregnancy (where plasma volume expands more than red blood cell mass, lowering hemoglobin concentration). Despite lower average hemoglobin, healthy women should still target 14.5-15.5 g/dL for optimal performance.
Can I have normal hemoglobin but still be iron deficient?
Yes, this is common. Iron deficiency develops progressively: first, ferritin (iron stores) depletes; then, iron available for hemoglobin production declines; finally, hemoglobin production falls. Many people experience fatigue, reduced exercise capacity, and other symptoms when ferritin is low (below 30-50 ng/mL) even when hemoglobin is still “normal.” Always check ferritin alongside hemoglobin to assess complete iron status.
Testing Hemoglobin With ApexBlood
ApexBlood’s comprehensive blood panel includes hemoglobin as part of the complete blood count (CBC), along with all related markers necessary to understand your oxygen-carrying capacity and red blood cell health: hematocrit (percentage of blood that is red blood cells), RBC count (number of red blood cells), MCV (mean corpuscular volume—red blood cell size), MCH (mean corpuscular hemoglobin), MCHC (mean corpuscular hemoglobin concentration), and RDW (red cell distribution width—variation in cell size).
Our testing also includes critical markers that reveal what’s driving your hemoglobin levels: ferritin (iron storage), iron and TIBC (total iron binding capacity) for iron status, vitamin B12 for red blood cell production, and complete metabolic markers to assess overall health affecting hemoglobin.
This comprehensive approach reveals not just your hemoglobin level but the complete picture—whether you have adequate iron stores to maintain optimal production, whether red blood cells are the right size and contain optimal hemoglobin, and whether any nutritional deficiencies are limiting oxygen-carrying capacity.
Most doctors check hemoglobin only when investigating anemia. But high performers understand that optimization requires measuring hemoglobin regularly alongside iron markers to ensure you’re operating at peak oxygen-carrying capacity, not just avoiding clinical disease.
You can’t optimize what you don’t measure. Stop accepting low-normal hemoglobin when optimal levels dramatically improve energy, performance, and cognitive function.
Get comprehensive testing including hemoglobin and iron markers – $189
The Bottom Line on Hemoglobin
Hemoglobin determines your oxygen-carrying capacity—the foundation of energy production, physical performance, and cognitive function. It’s not just about preventing anemia; it’s about optimizing the oxygen delivery system that powers every cell in your body.
Optimal hemoglobin for men is 15.0-17.0 g/dL, ideally 15.5-16.5 g/dL. For women, optimal is 14.0-16.0 g/dL, ideally 14.5-15.5 g/dL. These levels ensure maximum oxygen delivery to muscles, brain, and all tissues. Standard “normal” ranges include unhealthy populations and don’t represent optimal performance.
Low or low-normal hemoglobin (12-13.5 g/dL in men, 11.5-13 g/dL in women) causes fatigue, reduced exercise capacity, impaired cognitive function, and cold intolerance even when not technically “anemic.” The difference between low-normal and optimal hemoglobin is substantial—approximately 15-20% difference in oxygen-carrying capacity.
Optimizing hemoglobin requires ensuring adequate iron (check ferritin, target 50-100+ ng/mL), sufficient vitamin B12 (above 400-500 pg/mL) and folate, adequate protein intake, addressing any sources of blood loss, and reducing chronic inflammation that impairs production.
High performers don’t accept “within normal range” when normal includes sedentary, poorly nourished populations. They measure hemoglobin and related markers regularly, optimize iron status before hemoglobin declines, and maintain oxygen-carrying capacity at levels that support peak physical and cognitive performance.
Your cells need oxygen. Your mitochondria need oxygen. Your brain needs oxygen. Hemoglobin delivers it. Optimize accordingly.
Stop accepting suboptimal oxygen delivery when comprehensive testing and targeted optimization reveal your true potential. Stop accepting “normal” when optimal is possible.
Medical Disclaimer: This information is for educational purposes and does not constitute medical advice. Hemoglobin levels and red blood cell health require evaluation by qualified healthcare providers. Never make treatment decisions based solely on internet information. Always consult licensed medical professionals for diagnosis and treatment.
