High-Sensitivity C-Reactive Protein (hs-CRP): The Inflammation Marker That Predicts Your Health Decades in Advance
Your body is constantly sending signals about what’s happening beneath the surface. One of the most powerful predictive signals? High-sensitivity C-Reactive Protein, or hs-CRP. This biomarker doesn’t just tell you about inflammation happening right now. It tells you about cardiovascular events, metabolic dysfunction, and chronic disease risk years before symptoms appear.
Most people only hear about CRP when something has already gone wrong. A heart attack. An autoimmune flare. A chronic condition that’s been brewing for years. But high performers don’t wait for the check engine light. They monitor inflammation proactively, catch trends early, and optimize aggressively. That’s where hs-CRP testing becomes essential.
What Is High-Sensitivity C-Reactive Protein?
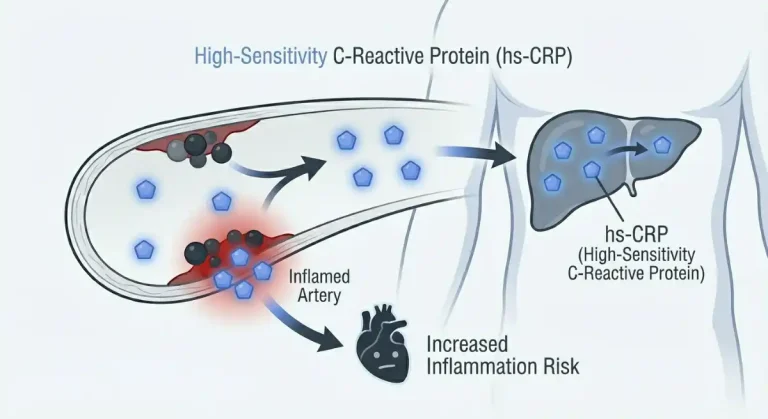
C-Reactive Protein is a protein produced by your liver in response to inflammation anywhere in your body. It’s part of your acute phase response, the immune system’s rapid reaction to injury, infection, or tissue damage. When inflammation rises, so does CRP.
The “high-sensitivity” version of the test (hs-CRP) measures very low levels of this protein with precision. While standard CRP tests are used to detect acute inflammation from infections or injuries, hs-CRP detects chronic, low-grade inflammation that silently damages your cardiovascular system, metabolism, and longevity potential.
This distinction matters enormously. Standard CRP might miss the subtle inflammatory state that’s quietly increasing your risk of heart disease by 200-300%. hs-CRP catches it.
Why hs-CRP Matters for Performance and Longevity
Chronic inflammation is the common thread connecting almost every disease of aging: cardiovascular disease, type 2 diabetes, Alzheimer’s, cancer, and accelerated biological aging itself. It’s not dramatic or acute. It’s the constant, low-level fire that damages tissues over decades.
For high performers, inflammation directly impacts:
Cognitive function: Chronic inflammation impairs memory, focus, and processing speed. Brain fog isn’t just poor sleep or stress. It’s often inflammatory.
Recovery capacity: Inflammation slows muscle recovery, increases injury risk, and limits training adaptations. You can’t optimize performance when your body is constantly in repair mode.
Energy and fatigue: Inflammatory cytokines directly cause fatigue by affecting mitochondrial function and energy production. That persistent tiredness isn’t necessarily burnout.
Cardiovascular risk: Elevated hs-CRP predicts heart attacks and strokes years in advance, independent of cholesterol levels. You can have perfect lipids and still be at high risk if inflammation is elevated.
Metabolic health: Inflammation drives insulin resistance, weight gain, and metabolic syndrome. It’s nearly impossible to optimize body composition when systemic inflammation is high.
Normal vs. Optimal hs-CRP Levels
Here’s where conventional medicine fails you.
Standard Reference Ranges:
- Low risk: Less than 1.0 mg/L
- Average risk: 1.0-3.0 mg/L
- High risk: Greater than 3.0 mg/L
The Problem With “Normal”:
These ranges were developed by looking at average populations, which means they include people with poor diets, sedentary lifestyles, obesity, and undiagnosed chronic conditions. “Average risk” in a sick population is still significant risk.
Furthermore, even within the “low risk” category, there’s meaningful variation. Someone at 0.9 mg/L isn’t in the same position as someone at 0.3 mg/L, even though both are technically “low risk.”
Optimal Range for Performance and Longevity:
For true optimization, you want hs-CRP below 0.5 mg/L, ideally below 0.3 mg/L. At these levels, you’re not just avoiding disease risk. You’re maximizing recovery, cognitive function, and healthspan.
Research consistently shows that people with hs-CRP below 1.0 mg/L have significantly lower cardiovascular event rates compared to those in the 1.0-3.0 range. But high performers shouldn’t settle for “lower risk.” The goal is minimized inflammation, maximized biology.
What Causes Elevated hs-CRP?
Multiple factors contribute to chronic inflammation:
Excess body fat, particularly visceral fat: Adipose tissue, especially around organs, actively secretes inflammatory cytokines. It’s not inert storage. It’s metabolically active and inflammatory.
Poor diet: Processed foods, excess sugar, refined carbohydrates, and seed oils high in omega-6 fatty acids all promote inflammation. The standard American diet is fundamentally inflammatory.
Chronic stress: Elevated cortisol and stress hormones trigger inflammatory pathways. Psychological stress translates directly into biological inflammation.
Poor sleep quality: Sleep deprivation increases inflammatory markers consistently. Even one night of poor sleep can elevate CRP.
Sedentary lifestyle: Lack of movement increases systemic inflammation. Paradoxically, excessive training without adequate recovery does the same.
Gut dysfunction: Intestinal permeability (“leaky gut”), dysbiosis, and inflammatory bowel conditions drive systemic inflammation through the gut-immune axis.
Chronic infections: Unresolved infections, including periodontal disease, can maintain elevated CRP for years.
Autoimmune conditions: Conditions like rheumatoid arthritis, lupus, and inflammatory bowel disease cause persistent elevation.
Smoking and alcohol: Both directly increase inflammatory markers throughout the body.
Symptoms and Consequences of Elevated hs-CRP
The insidious aspect of chronic inflammation is that it often operates silently. You might not feel acutely sick, but the damage accumulates.
Common manifestations include persistent fatigue that doesn’t improve with rest, brain fog and reduced cognitive clarity, poor recovery from workouts or physical stress, increased susceptibility to infections, unexplained joint or muscle aches, difficulty losing weight despite dietary efforts, and mood changes including depression and anxiety.
Long-term consequences are far more serious. Elevated hs-CRP independently predicts cardiovascular events including heart attack and stroke, even when cholesterol is normal. It’s associated with increased risk of type 2 diabetes and metabolic syndrome, accelerated cognitive decline and dementia risk, higher cancer incidence across multiple types, faster biological aging at the cellular level, and increased all-cause mortality.
You can’t optimize what you don’t measure. Most people discover their inflammation problem only after a major health event. High performers test proactively.
How to Lower hs-CRP
Reducing chronic inflammation requires a comprehensive approach targeting multiple pathways simultaneously.
Dietary interventions form the foundation. Eliminate or dramatically reduce processed foods, refined sugars, and excess omega-6 fatty acids from seed oils. Increase omega-3 fatty acids from fatty fish, quality fish oil, or algae supplements. Emphasize anti-inflammatory foods like colorful vegetables, berries, leafy greens, nuts, seeds, and olive oil. Consider removing common inflammatory triggers like gluten or dairy if you suspect sensitivity.
Body composition optimization is often essential. Reducing excess body fat, particularly visceral fat, directly lowers inflammatory cytokine production. This isn’t just aesthetic. It’s metabolic necessity.
Exercise with appropriate recovery provides powerful anti-inflammatory effects, but only when properly balanced. Moderate-intensity regular exercise consistently lowers CRP. However, excessive training without adequate recovery can increase inflammation. The dose makes the poison.
Sleep optimization is non-negotiable. Aim for 7-9 hours of quality sleep nightly. Sleep deprivation reliably increases inflammatory markers within days.
Stress management through meditation, breathwork, therapy, or other evidence-based practices directly reduces inflammatory signaling. Chronic psychological stress translates into chronic biological inflammation.
Gut health optimization through diverse fiber intake, fermented foods, and potentially targeted probiotics can reduce systemic inflammation originating from intestinal dysfunction.
Address chronic infections including periodontal disease, which is often overlooked but significantly impacts systemic inflammation.
hs-CRP and Other Health Markers
hs-CRP doesn’t exist in isolation. It interacts with and influences numerous other biomarkers.
Lipid markers: Inflammation oxidizes LDL cholesterol, making it more atherogenic. You can have moderately elevated LDL that’s relatively harmless if inflammation is low, or you can have LDL in “normal” range that’s highly dangerous if inflammation is high. Context matters.
Insulin and glucose metabolism: Inflammation drives insulin resistance. Elevated hs-CRP often precedes metabolic dysfunction, making it an early warning signal for diabetes risk.
Homocysteine: Both are cardiovascular risk markers that often elevate together, particularly in the presence of poor B-vitamin status or genetic factors like MTHFR mutations.
Fibrinogen: Another inflammatory marker that, combined with elevated hs-CRP, significantly increases thrombotic risk.
White blood cell count: General immune activation often correlates with elevated hs-CRP, particularly when chronic infection or autoimmune activity is present.
Liver enzymes: Since CRP is produced in the liver, liver function affects CRP production. Conversely, systemic inflammation can impact liver health.
hs-CRP and Longevity Optimization
Chronic inflammation accelerates biological aging at the cellular level. Inflammatory cytokines shorten telomeres, impair mitochondrial function, promote cellular senescence, and activate pathways that speed aging.
Longevity isn’t just about living longer. It’s about extending healthspan, the years you’re physically and cognitively capable. Inflammation compresses healthspan by accelerating the transition from vitality to frailty.
For individuals pursuing longevity optimization, hs-CRP below 0.5 mg/L should be a baseline target. This often requires combining dietary optimization, body composition management, and strategic interventions.
Frequently Asked Questions
How often should I test hs-CRP?
For baseline assessment, include it in comprehensive annual bloodwork. If elevated, retest every 3-6 months while implementing interventions to track progress. Once optimized, annual testing is typically sufficient unless risk factors change.
Can hs-CRP be too low?
Extremely low levels (undetectable) are generally not concerning. Unlike some biomarkers where too low creates problems, very low hs-CRP simply indicates minimal inflammation, which is ideal for longevity and performance.
What if my hs-CRP is elevated but I feel fine?
This is precisely why testing matters. Chronic inflammation operates silently for years before symptoms appear. Feeling fine doesn’t mean your biology is optimized. Elevated hs-CRP is a warning signal to address inflammation before it causes irreversible damage.
Can acute illness affect hs-CRP?
Yes. Acute infections, injuries, or inflammatory episodes will spike CRP dramatically. If you’re acutely sick, wait 2-3 weeks after recovery before testing hs-CRP for an accurate baseline assessment.
Is hs-CRP different from regular CRP?
Yes. Standard CRP tests measure higher ranges (typically 3-100+ mg/L) used for detecting acute inflammation from infections or injuries. hs-CRP measures much lower levels (0.1-10 mg/L) that predict chronic disease risk. The hs-CRP test is far more valuable for performance and longevity optimization.
Do medications affect hs-CRP?
Statins, certain blood pressure medications, and anti-inflammatory drugs can lower CRP. This doesn’t mean the underlying inflammation is resolved, just that it’s being suppressed. Address root causes rather than masking markers.
Can stress alone elevate hs-CRP?
Absolutely. Chronic psychological stress directly increases inflammatory markers through cortisol dysregulation and immune activation. Mental health is biological health.
What’s the fastest way to lower hs-CRP?
There’s no magic bullet, but combining anti-inflammatory diet changes, reducing excess body fat, optimizing sleep, and managing stress typically produces measurable improvements within 6-12 weeks. Consistency matters more than any single intervention.
Testing hs-CRP With ApexBlood
hs-CRP is included in ApexBlood’s comprehensive blood panel alongside 100+ other biomarkers that provide complete context for your health and performance. Inflammation doesn’t exist in a vacuum. It affects and is affected by hormones, metabolism, cardiovascular markers, liver function, and more.
Understanding your hs-CRP in context with your complete biological profile allows for targeted, effective interventions rather than guesswork. You can’t optimize what you don’t measure, and you can’t understand one marker without seeing the complete picture.
Get comprehensive testing for $189
The Bottom Line on hs-CRP
High-sensitivity C-Reactive Protein is one of the most predictive biomarkers available for long-term health outcomes. It tells you about cardiovascular risk, metabolic dysfunction, and biological aging years before symptoms appear.
Your doctor might tell you that 2.5 mg/L is “normal” because it falls within reference ranges. But normal for a sick population isn’t optimal for performance and longevity. You should be targeting below 0.5 mg/L, ideally below 0.3 mg/L.
Chronic inflammation silently damages your body for decades before manifesting as disease. By the time you feel it, significant damage has occurred. High performers test proactively, identify inflammation early, and address it aggressively through diet, lifestyle, body composition, and when appropriate, medical interventions.
You can’t optimize what you don’t measure. Stop accepting “normal” when optimal is possible.
Medical Disclaimer: This information is for educational purposes and does not constitute medical advice. High-sensitivity C-Reactive Protein and inflammation require evaluation by qualified healthcare providers. Never make treatment decisions based solely on internet information. Always consult licensed medical professionals for diagnosis and treatment.
