VLDL Cholesterol: The Forgotten Lipid Marker That Reveals Your Metabolic Truth
When people talk about cholesterol, the conversation inevitably centers on LDL (the “bad” cholesterol) and HDL (the “good” cholesterol). But there’s a third player that rarely gets attention despite being one of the most revealing markers of metabolic health: VLDL cholesterol.
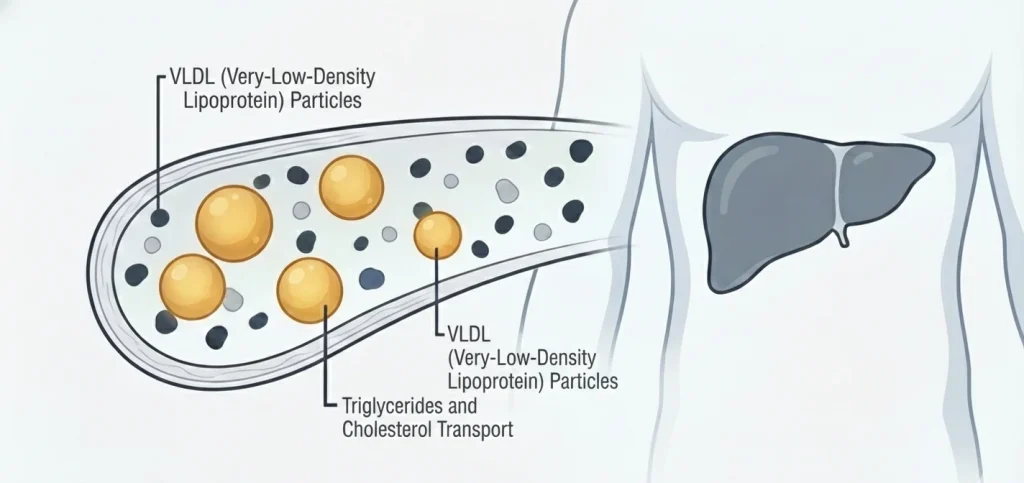
VLDL—very low-density lipoprotein—is the triglyceride-rich particle your liver produces to transport fat throughout your body. When VLDL is elevated, it’s not just a cholesterol problem. It’s a metabolic dysfunction problem. High VLDL signals that your liver is overproducing fat, your body can’t efficiently clear it from your bloodstream, and you’re likely on the path toward insulin resistance, fatty liver disease, and cardiovascular complications.
Most doctors don’t even discuss VLDL with patients because it’s typically calculated rather than directly measured, and it’s overshadowed by LDL in cardiovascular risk discussions. But for anyone serious about metabolic optimization, VLDL deserves close attention. It’s the canary in the coal mine for metabolic dysfunction—often elevated years before diabetes, heart disease, or other serious conditions develop.
What Is VLDL Cholesterol?
VLDL is a lipoprotein particle produced by your liver to transport triglycerides (fat) from the liver to peripheral tissues where it’s either used for energy or stored in fat cells. Think of VLDL as the delivery truck that carries fat from the manufacturing plant (your liver) to various locations throughout your body.
VLDL particles are composed primarily of triglycerides (55-65%), with smaller amounts of cholesterol (10-15%), phospholipids, and proteins. As VLDL particles circulate through your bloodstream, enzymes break down the triglycerides, releasing them to tissues. As triglycerides are removed, VLDL particles shrink and eventually transform into IDL (intermediate-density lipoprotein) and then LDL particles.
This is why VLDL, triglycerides, and LDL are intimately connected. High VLDL production means high triglyceride levels and often leads to increased small, dense LDL particles—the most atherogenic (artery-clogging) type of LDL.
VLDL cholesterol is typically calculated rather than directly measured in standard lipid panels. The standard formula is: VLDL = Triglycerides ÷ 5 (when measured in mg/dL). This calculation is reasonably accurate when triglycerides are below 400 mg/dL, but becomes less reliable at very high triglyceride levels.
Why VLDL Matters for Metabolic Health
VLDL is fundamentally a metabolic marker disguised as a lipid measurement. Elevated VLDL doesn’t just indicate cardiovascular risk—it reveals how efficiently your body processes energy, manages blood sugar, and responds to insulin.
VLDL reflects hepatic fat production. When your liver produces excessive VLDL, it indicates the liver is either receiving too much substrate (excess carbohydrates, calories, or alcohol) or is metabolically dysfunctional and overproducing fat regardless of input. This is often the first sign of non-alcoholic fatty liver disease (NAFLD), which affects up to 30% of adults in developed countries.
VLDL indicates insulin resistance. Insulin normally suppresses VLDL production by the liver. When cells become insulin resistant, this suppression fails, and the liver churns out VLDL even when it shouldn’t. High VLDL is therefore a direct marker of hepatic insulin resistance—often appearing before fasting glucose or hemoglobin A1c become abnormal.
VLDL promotes atherogenic LDL particles. As VLDL particles lose their triglycerides and transform into LDL, they create small, dense LDL particles that easily penetrate arterial walls and become oxidized, driving atherosclerosis. High VLDL means you’re producing more of these dangerous LDL particles, dramatically increasing cardiovascular risk even when total LDL cholesterol looks “normal.”
VLDL correlates with metabolic syndrome. Elevated VLDL is a core feature of metabolic syndrome alongside abdominal obesity, high blood pressure, elevated fasting glucose, and low HDL cholesterol. If your VLDL is high, you likely have at least one other component of metabolic syndrome, and you’re at significantly increased risk for type 2 diabetes and cardiovascular disease.
VLDL reflects dietary and lifestyle patterns. Unlike genetic forms of high cholesterol, VLDL is primarily driven by modifiable factors: excess carbohydrate intake (particularly refined carbs and sugar), alcohol consumption, sedentary lifestyle, obesity and visceral fat accumulation, and poor sleep and chronic stress. This makes VLDL both a warning signal and an opportunity—it reveals problems early while they’re still reversible through lifestyle intervention.
Normal vs. Optimal VLDL Levels
Here’s where conventional medicine provides inadequate guidance.
Standard Reference Ranges:
- Normal: 2-30 mg/dL
- Borderline: 31-40 mg/dL
- High: Above 40 mg/dL
The Problem With “Normal”:
These ranges are absurdly broad and based on population averages that include widespread metabolic dysfunction. Someone at 30 mg/dL is considered “normal” despite being at the upper limit where metabolic problems often begin. Meanwhile, someone at 5 mg/dL and someone at 29 mg/dL are treated as equivalent despite vastly different metabolic states.
Most doctors don’t even mention VLDL unless it’s dramatically elevated above 40 mg/dL, by which point significant metabolic dysfunction has been present for years. This reactive approach waits for disease rather than optimizing for health.
Optimal Range for Performance and Longevity:
For true metabolic health, VLDL should be below 15 mg/dL, ideally below 10 mg/dL. At these levels, you’re demonstrating efficient fat metabolism, good insulin sensitivity, minimal hepatic fat production, and low production of atherogenic LDL particles.
Since VLDL is calculated from triglycerides (VLDL = Triglycerides ÷ 5), optimal VLDL below 10 mg/dL corresponds to triglycerides below 50 mg/dL—a level that indicates excellent metabolic health and insulin sensitivity.
Research consistently shows that people with lower VLDL and triglycerides have better insulin sensitivity, lower cardiovascular event rates, reduced fatty liver prevalence, and improved longevity markers compared to those in the “normal” range of 20-30 mg/dL.
Your doctor might say VLDL at 28 mg/dL is “fine.” For disease avoidance in a metabolically sick population, maybe. For optimal metabolic health and performance? You’re operating at significantly suboptimal capacity.
What Causes Elevated VLDL?
VLDL elevation is almost always metabolic and lifestyle-driven, making it both concerning (it reveals dysfunction) and encouraging (it’s largely reversible).
Excess carbohydrate intake is the primary driver of elevated VLDL. When you consume more carbohydrates than your body can immediately use or store as glycogen, the liver converts excess glucose into triglycerides and packages them into VLDL particles for export. Chronically high carbohydrate intake—particularly from refined grains, sugar, and processed foods—keeps VLDL production elevated. This is why low-carbohydrate diets so consistently lower VLDL and triglycerides.
Insulin resistance creates a vicious cycle. When hepatic cells become resistant to insulin’s signal, the liver fails to suppress VLDL production appropriately. High insulin levels (which occur when you’re insulin resistant) simultaneously tell the liver to produce more VLDL while preventing fat cells from releasing stored triglycerides. The result is elevated blood VLDL and triglycerides despite expanding fat stores.
Alcohol consumption dramatically increases VLDL production. The liver prioritizes alcohol metabolism over other processes, disrupting normal fat metabolism and leading to increased VLDL synthesis. Even moderate drinking elevates VLDL in susceptible individuals. Heavy drinking consistently produces high VLDL and triglycerides alongside fatty liver disease.
Obesity and visceral fat aren’t just inert storage—visceral adipose tissue actively releases fatty acids that flood to the liver, providing substrate for increased VLDL production. The more visceral fat you carry, the more VLDL your liver typically produces.
Poor diet quality beyond just carbohydrates matters. Diets high in omega-6 fatty acids from seed oils (soybean, corn, canola) and processed foods promote inflammation and worsen metabolic dysfunction, increasing VLDL production. Trans fats and oxidized oils from fried and processed foods dramatically worsen lipid profiles including VLDL.
Sedentary lifestyle reduces the body’s ability to clear VLDL and triglycerides from the bloodstream. Regular physical activity improves VLDL clearance and reduces hepatic VLDL production, while inactivity has the opposite effect.
Sleep deprivation and poor sleep quality disrupt metabolic hormones, worsen insulin resistance, and increase VLDL production. Even a few nights of inadequate sleep measurably elevates VLDL and triglycerides.
Chronic stress elevates cortisol, which promotes hepatic glucose production, insulin resistance, and increased VLDL synthesis. The stress-VLDL-metabolic dysfunction connection is significant and often overlooked.
Type 2 diabetes and prediabetes are characterized by elevated VLDL production due to severe insulin resistance. The metabolic dysfunction driving diabetes directly causes VLDL overproduction.
Certain medications including corticosteroids, some beta-blockers, thiazide diuretics, and estrogen can elevate VLDL as a side effect.
Genetic factors play a smaller role than with LDL cholesterol, but some genetic variations affect VLDL metabolism. However, even with genetic predisposition, lifestyle factors remain the primary determinant of VLDL levels.
The VLDL-Triglyceride-LDL Connection
Understanding the relationship between VLDL, triglycerides, and LDL is essential for grasping metabolic health.
VLDL carries triglycerides. When you see elevated triglycerides on your lipid panel, you’re seeing elevated VLDL. They rise and fall together because VLDL is the primary carrier of triglycerides in your bloodstream. VLDL = Triglycerides ÷ 5 makes this mathematical relationship explicit.
VLDL becomes LDL. As VLDL particles circulate, enzymes (lipoprotein lipase) break down triglycerides and release them to tissues. As VLDL loses triglycerides, it shrinks and transforms first into IDL (intermediate-density lipoprotein) and then into LDL particles. High VLDL production means more LDL particles are eventually created.
High VLDL creates dangerous LDL particles. When VLDL and triglycerides are elevated, the LDL particles produced tend to be small and dense—the type that easily penetrates arterial walls, becomes oxidized, and drives atherosclerosis. This is why someone with “normal” total LDL cholesterol can still be at high cardiovascular risk if their VLDL and triglycerides are elevated—the LDL particles are the dangerous small, dense type.
The atherogenic dyslipidemia triad consists of high triglycerides (and therefore high VLDL), low HDL cholesterol, and small dense LDL particles. This lipid pattern is extremely atherogenic (artery-clogging) and dramatically increases cardiovascular risk. It’s the characteristic lipid profile of insulin resistance and metabolic syndrome. VLDL is at the center of this dangerous pattern.
VLDL affects HDL metabolism. High VLDL and triglycerides interfere with HDL metabolism, often lowering protective HDL cholesterol. The enzymes that process VLDL also affect HDL particles, and when overwhelmed by excessive VLDL, HDL levels typically decline. This is why high triglycerides and low HDL so often appear together.
Lowering VLDL through diet and lifestyle improvements simultaneously lowers triglycerides, reduces small dense LDL production, and often raises HDL—comprehensively improving your entire lipid profile from a single intervention.
VLDL and Fatty Liver Disease
Elevated VLDL and non-alcoholic fatty liver disease (NAFLD) are intimately connected. In fact, VLDL elevation is often the first detectable sign that fat is accumulating in your liver.
When the liver accumulates excess fat (from excess carbohydrates, alcohol, obesity, or insulin resistance), it attempts to export that fat by producing more VLDL. Initially, this compensatory mechanism prevents extreme fat buildup. But over time, the liver becomes overwhelmed—it can’t export fat fast enough, leading to progressive hepatic steatosis (fatty liver).
The progression looks like this: excess substrate (carbs, calories, alcohol) leads to increased hepatic triglyceride synthesis, liver exports fat as VLDL (visible as high VLDL and triglycerides in bloodwork), eventually the liver can’t keep up and fat accumulates (fatty liver develops), fatty liver causes inflammation and insulin resistance, worsening insulin resistance further increases VLDL production, and the cycle accelerates toward metabolic dysfunction, cirrhosis, and liver failure if unchecked.
Elevated VLDL (above 20 mg/dL) with elevated liver enzymes (ALT, AST) strongly suggests fatty liver requiring intervention. Even without elevated liver enzymes, high VLDL indicates excessive hepatic fat production and likely some degree of fatty infiltration.
The good news? NAFLD is often reversible with weight loss, carbohydrate reduction, alcohol elimination, exercise, and metabolic optimization. As fatty liver improves, VLDL production normalizes, creating a positive feedback loop of metabolic recovery.
How to Lower VLDL Cholesterol
Lowering VLDL requires addressing the metabolic dysfunction driving its overproduction. The interventions that lower VLDL are the same ones that reverse insulin resistance, reduce fatty liver, and optimize metabolic health.
Reduce refined carbohydrates and sugar aggressively. This is the single most effective dietary intervention for lowering VLDL. Eliminate or dramatically reduce sugary beverages, desserts, candy, and sweetened foods, refined grains (white bread, white rice, pasta, most baked goods), and processed foods high in added sugars. For many people, adopting a lower-carbohydrate approach (100-150g carbs daily or less) produces dramatic VLDL and triglyceride reductions within weeks.
Eliminate or limit alcohol consumption. Alcohol is one of the most potent drivers of VLDL production. Even moderate drinking (2-3 drinks daily) significantly elevates VLDL in many people. Heavy drinking consistently produces very high VLDL alongside fatty liver disease. If your VLDL is elevated, eliminating alcohol for 4-8 weeks and retesting often produces dramatic improvements.
Optimize protein and fat intake. Increase protein intake to support satiety and metabolic health. Emphasize healthy fats from olive oil, avocados, nuts, seeds, and fatty fish. These fats don’t increase VLDL production the way excess carbohydrates do. Omega-3 fatty acids from fatty fish or quality supplements directly reduce hepatic VLDL production and triglyceride synthesis.
Lose weight, particularly visceral fat. Even modest weight loss (5-10% of body weight) significantly reduces VLDL production. Visceral fat reduction is particularly important because visceral adipose tissue directly floods the liver with fatty acids, driving VLDL synthesis. As visceral fat decreases, hepatic VLDL production normalizes.
Exercise consistently. Both aerobic exercise and resistance training improve VLDL clearance from the bloodstream and reduce hepatic VLDL production. Aim for at least 150 minutes of moderate-intensity activity weekly, though more is often better. High-intensity interval training appears particularly effective for improving metabolic health and reducing VLDL.
Improve sleep quality. Prioritize 7-9 hours of quality sleep nightly. Sleep deprivation reliably increases VLDL and triglycerides within days, while sleep restoration improves them. This isn’t optional—sleep is metabolically essential.
Manage stress effectively. Chronic stress elevates cortisol and worsens insulin resistance, driving VLDL overproduction. Evidence-based stress management (meditation, breathwork, therapy, adequate recovery) directly improves metabolic health and reduces VLDL.
Address insulin resistance directly. Since insulin resistance is often the root cause of elevated VLDL, interventions that improve insulin sensitivity provide comprehensive benefits. All of the above strategies improve insulin sensitivity, creating a positive feedback loop where better insulin sensitivity further reduces VLDL production.
VLDL and Metabolic Optimization Treatments
When lifestyle interventions alone are insufficient to normalize VLDL, or when metabolic dysfunction is severe, targeted medical treatments can support VLDL reduction alongside continued lifestyle optimization.
Metformin improves insulin sensitivity at the cellular level, which directly reduces hepatic VLDL production. By improving how the liver responds to insulin’s signal to suppress fat production, metformin often produces significant VLDL and triglyceride reductions. This is particularly effective when insulin resistance is the primary driver of elevated VLDL. Studies consistently show metformin reduces triglycerides by 10-20% on average, which corresponds to similar VLDL reductions.
Weight loss medications including GLP-1s (semaglutide, tirzepatide) produce dramatic VLDL improvements as patients lose significant weight and reverse metabolic dysfunction. As visceral fat decreases and insulin sensitivity improves, hepatic VLDL production normalizes. Patients often see VLDL and triglycerides drop by 30-50% or more as they achieve substantial weight loss. The metabolic improvements from weight loss often persist even after medication is discontinued if healthy lifestyle patterns are maintained.
Hormone optimization may support healthy VLDL levels when hormonal imbalances contribute to metabolic dysfunction. Low testosterone in men is associated with insulin resistance, visceral fat accumulation, and elevated VLDL and triglycerides. Optimizing testosterone often improves insulin sensitivity and body composition, which can reduce VLDL production. In women, hormonal changes during perimenopause and menopause typically worsen lipid profiles including VLDL elevation, and hormone optimization may provide metabolic benefits.
These medical interventions work synergistically with dietary optimization, exercise, sleep, and stress management to comprehensively address the metabolic dysfunction driving VLDL overproduction. They’re tools that amplify lifestyle efforts, not replacements for them.
VLDL and Cardiovascular Risk
While LDL cholesterol gets most of the attention in cardiovascular risk discussions, VLDL is an independent and powerful predictor of heart disease and stroke.
VLDL remnants are highly atherogenic. As VLDL particles lose triglycerides, they become smaller and denser, eventually forming IDL and LDL particles. During this process, VLDL remnants—partially metabolized VLDL particles—accumulate in the bloodstream when clearance is impaired. These remnants easily penetrate arterial walls and contribute directly to atherosclerotic plaque formation. In some studies, VLDL remnants are even more atherogenic than LDL particles.
High VLDL indicates metabolic syndrome. Metabolic syndrome dramatically increases cardiovascular risk—people with metabolic syndrome have 2-3 times higher risk of heart disease and stroke compared to those without it. Elevated VLDL is a core feature of metabolic syndrome and signals the presence of multiple cardiovascular risk factors simultaneously.
VLDL promotes inflammation. Elevated VLDL and triglycerides increase oxidative stress and inflammation in blood vessels, damaging endothelial function and promoting plaque formation. This inflammatory process is central to cardiovascular disease development.
VLDL correlates with insulin resistance. Insulin resistance itself is a major cardiovascular risk factor independent of lipid levels. High VLDL indicates insulin resistance, which means cardiovascular risk is elevated even beyond what the lipid numbers alone suggest.
VLDL creates dangerous LDL particles. High VLDL production leads to increased small, dense LDL particles that are far more atherogenic than large, fluffy LDL. Even when total LDL cholesterol appears “normal,” if VLDL is elevated, the LDL particles are likely the dangerous type.
Comprehensive cardiovascular risk assessment should always include VLDL (or triglycerides, which reflect VLDL) alongside LDL, HDL, inflammatory markers like hs-CRP, insulin and glucose markers, and blood pressure. VLDL elevation is a red flag demanding attention, not a secondary concern overshadowed by LDL.
VLDL vs. LDL: Which Matters More?
This is the wrong question—both matter, but they reveal different things about your health.
LDL cholesterol indicates the total amount of cholesterol carried in LDL particles. It’s influenced by genetics (some people naturally produce more LDL), diet (particularly saturated fat in genetically susceptible individuals), and metabolic factors. LDL is strongly associated with cardiovascular risk, particularly when LDL particles are small and dense.
VLDL cholesterol indicates hepatic fat production and insulin sensitivity. It’s primarily driven by modifiable lifestyle factors (carbohydrate intake, alcohol, obesity, inactivity). VLDL is a metabolic dysfunction marker that predicts not just cardiovascular disease but also diabetes, fatty liver, and metabolic syndrome.
The key difference: LDL can be elevated in otherwise metabolically healthy people due to genetic factors. High LDL with low VLDL, low triglycerides, and high HDL often indicates large, fluffy LDL particles with lower cardiovascular risk. In contrast, high VLDL almost always indicates metabolic dysfunction regardless of genetics. High VLDL signals insulin resistance, fatty liver, and atherogenic dyslipidemia even when total LDL appears “normal.”
The dangerous combination is elevated LDL AND elevated VLDL together, which indicates both genetic/dietary factors affecting LDL production and metabolic dysfunction driving VLDL overproduction. This combination creates maximal cardiovascular risk.
For metabolic health assessment, VLDL (and triglycerides) provide more useful information than LDL alone. A comprehensive lipid panel should always consider both, along with HDL, to understand true cardiovascular and metabolic risk.
Frequently Asked Questions
What is a normal VLDL cholesterol level?
Standard reference ranges consider VLDL below 30 mg/dL “normal,” but optimal for metabolic health is below 15 mg/dL, ideally below 10 mg/dL. At these levels, you’re demonstrating efficient fat metabolism, good insulin sensitivity, and minimal hepatic fat overproduction. VLDL above 20 mg/dL suggests suboptimal metabolic health worth addressing proactively.
How is VLDL different from LDL?
VLDL and LDL are both lipoproteins that carry cholesterol, but they differ significantly. VLDL is produced by the liver and primarily carries triglycerides (fat), while LDL is created from VLDL after triglycerides are removed and primarily carries cholesterol. VLDL is much larger and less dense than LDL. As VLDL particles lose triglycerides, they transform into LDL particles. VLDL is driven primarily by metabolic factors (carbs, insulin resistance, alcohol), while LDL is influenced more by genetics and dietary cholesterol/saturated fat.
Can you have high VLDL with normal LDL?
Yes, this is common and indicates metabolic dysfunction. High VLDL with normal or even low LDL typically occurs when carbohydrate intake is high, insulin resistance is present, and alcohol consumption is significant. This pattern suggests the liver is overproducing VLDL but rapidly converting it to LDL and clearing it. However, the LDL particles produced are likely small and dense (dangerous), and cardiovascular risk is still elevated despite “normal” LDL numbers.
How quickly can you lower VLDL?
VLDL responds rapidly to dietary changes—faster than any other lipid marker. Aggressive carbohydrate reduction and alcohol elimination can lower VLDL by 30-50% within 2-4 weeks. Weight loss, exercise, and improved sleep produce additional reductions over 2-3 months. VLDL’s rapid response to lifestyle interventions makes it an excellent marker for tracking metabolic improvements.
Does VLDL cause fatty liver or does fatty liver cause VLDL?
It works both ways, creating a vicious cycle. Initially, excess substrate (carbs, alcohol, calories) causes the liver to produce more VLDL as it attempts to export fat. As the liver becomes overwhelmed and fat accumulates (fatty liver develops), the fatty liver causes inflammation and insulin resistance, which further increases VLDL production. Breaking this cycle requires addressing both dietary inputs and metabolic dysfunction simultaneously.
Is VLDL measured directly or calculated?
In standard lipid panels, VLDL is calculated using the formula: VLDL = Triglycerides ÷ 5 (when measured in mg/dL). This calculation is reasonably accurate when triglycerides are below 400 mg/dL. Advanced lipid testing can directly measure VLDL particles using specialized techniques like NMR spectroscopy, which provides more precise information but is more expensive and not typically included in routine testing.
What’s worse: high VLDL or high LDL?
Both are concerning but indicate different problems. High VLDL indicates metabolic dysfunction (insulin resistance, fatty liver, poor diet) and is almost always modifiable through lifestyle changes. High LDL can be genetic or dietary and may or may not indicate metabolic problems. From a metabolic health perspective, high VLDL is more concerning because it signals systemic dysfunction affecting multiple aspects of health beyond just cardiovascular risk. Ideally, both should be optimized.
Can medications lower VLDL?
Yes. Medications that improve insulin sensitivity (like metformin) reduce VLDL production. Fibrates (like fenofibrate) specifically target VLDL and triglyceride reduction and can lower VLDL by 30-50%. High-dose omega-3 prescriptions (like Vascepa or Lovaza) reduce VLDL and triglycerides significantly. Statins primarily target LDL but also modestly reduce VLDL. However, lifestyle interventions (carb reduction, weight loss, exercise) are typically more effective for VLDL reduction than medications alone.
Testing VLDL With ApexBlood
VLDL is included in ApexBlood’s comprehensive blood panel as part of the standard lipid assessment. However, understanding VLDL requires context from other metabolic markers including triglycerides (which directly determine calculated VLDL), HDL and LDL cholesterol, insulin and glucose for assessing insulin resistance, liver enzymes (ALT, AST) to evaluate fatty liver, and inflammatory markers like hs-CRP.
VLDL doesn’t exist in isolation—it’s part of a comprehensive metabolic picture that reveals how efficiently your body processes energy, handles blood sugar, and manages fat metabolism.
If you want advanced lipid testing beyond standard panels—direct VLDL particle measurement via NMR, LDL particle size and number, apolipoprotein B, remnant cholesterol, or other specialized cardiovascular markers—our physicians have access to over 2,000 lab partners nationwide and can order virtually any test available. Schedule a free consultation with our care team to discuss custom blood panel options at competitive pricing.
Get comprehensive testing for $189
The Bottom Line on VLDL Cholesterol
VLDL is the forgotten lipid marker that reveals metabolic truth. While everyone obsesses over LDL cholesterol, VLDL quietly signals insulin resistance, fatty liver, and metabolic dysfunction years before serious disease develops.
Elevated VLDL (above 20 mg/dL) isn’t just a cholesterol problem—it’s a metabolic problem. It indicates your liver is overproducing fat, your body can’t efficiently clear it, and you’re likely heading toward insulin resistance, diabetes, cardiovascular disease, and accelerated aging.
The good news? VLDL responds dramatically to lifestyle interventions. Carbohydrate reduction, alcohol elimination, weight loss, and exercise often normalize VLDL within weeks to months. Unlike genetic forms of high cholesterol that may require medication regardless of lifestyle, VLDL elevation is largely reversible through addressing root causes.
Your doctor probably doesn’t mention VLDL because it’s overshadowed by LDL and considered a secondary marker. But for anyone pursuing metabolic optimization and longevity, VLDL deserves close attention. It’s an early warning system for metabolic dysfunction—catch it early, address it aggressively, and prevent the cascade of metabolic disease before it starts.
You can’t optimize what you don’t measure. Stop accepting “normal” VLDL when optimal is possible.
Medical Disclaimer: This information is for educational purposes and does not constitute medical advice. VLDL cholesterol and metabolic health require evaluation by qualified healthcare providers. Never make treatment decisions based solely on internet information. Always consult licensed medical professionals for diagnosis and treatment.
